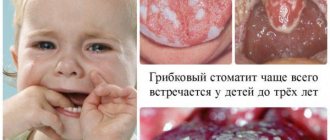
Infectious and inflammatory diseases of the oral cavity are often diagnosed in children. Doctors explain this by insufficient hygiene in childhood and the incomplete formation of the immune system.
In this case, it is necessary to distinguish between dangerous infections and benign inflammatory processes. Thus, temperature during stomatitis in children may indicate the infectious nature of the disease.
What is stomatitis
Stomatitis is an inflammatory process on the oral mucosa
In the medical literature, stomatitis is an inflammatory disease of the oral mucosa, characterized by the appearance of small white ulcers on the inner surface of the lips, gums, tongue and throat.
Depending on the cause, it may be aphthous or infectious stomatitis. The pathology is manifested by pain, general malaise and other symptoms.
The mucous membrane of epithelial origin covers almost the entire surface of the oral cavity. Special cells of the mucous membrane not only protect internal tissues, but also secrete various substances. Also in the oral cavity there are salivary glands necessary to ensure primary digestive functions.
When an ulcer occurs, the mucous membrane is damaged and the function of the surface epithelium is disrupted. As a rule, the disease has a benign course, but in rare cases dangerous complications may develop.
Small ulcers with stomatitis may appear during the day. Even without treatment, the inflammatory process is self-limiting within 7-10 days. However, large ulcers often require long-term treatment.
Stomatitis can also become chronic. In this case, foci of inflammation will appear periodically in different parts of the oral mucosa. Untimely or incorrect treatment contributes to relapses.
Candidal stomatitis in children (infants)
Cause
This type of stomatitis appears due to fungi, which are constantly present in the microflora of the oral cavity, but usually do not manifest themselves. Against the background of microflora disturbance (due to licking dirty toys, treatment of other diseases with antibiotics, acute respiratory infections, acute respiratory viral infections, during treatment with corticosteroids and other drugs that suppress the immune system, as well as with a high-carbohydrate diet), the growth of fungi of the genus Candida, which is the cause of stomatitis, is activated in infants.
Symptoms
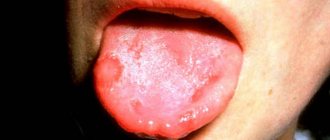
- a whitish or yellowish cheesy coating on the tongue, cheeks, and gums, which is easily removed. It is important to remember that young children who are breastfed and whose diet is dominated by dairy products may have a coating of milk on their tongue - this is normal and does not need to be treated.
- when removing plaque, the mucous membrane is swollen, slightly red, and may be painful.
General health is usually unchanged.
When it becomes chronic, dryness and pain occur in the mucous membranes, and swallowing is difficult.
Treatment
- Candida mushrooms are well preserved in the external environment. It is necessary to wash all toys, bottles, dishes, pacifiers and other objects with which the child comes into contact with soap or soda.
- In the oral cavity, plaque is easily removed with a solution of soda (1 teaspoon of soda per glass of cold boiled water) - use a gauze swab to wipe the areas where there is plaque.
- Antiseptics (furacilin, decoctions of medicinal herbs, chlorhexidine) - rinsing or wiping the mucous membrane 3 times a day.
- Diet correction (exclude sweet, spicy, sour foods as much as possible).
- Local antifungal drugs (cholisal - spread on the mucous membrane 3 times a day after removing plaque, hexoral - dissolve a tablet (for children over 4 years old) and others). Carefully read the instructions for use and age restrictions.
- If improvement does not occur within 3-4 days, then you should consult a doctor to prescribe antifungal drugs for general treatment, as well as to identify possible concomitant pathologies.
Types of pathology
Temperature with stomatitis in children
Stomatitis is classified according to the form of its course, source of occurrence and characteristic features. Main types:
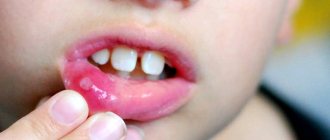
- Aphthous stomatitis is the appearance of ulcers of an inflammatory nature. This is the most common form of pathology among children. Signs include the appearance of sores that are pale white or yellowish in color with a red outer ring in the mouth. This may be one formation or several ulcers at once in different areas. Typical places of occurrence are the tissues of the inner lips and cheeks. Painful sensations are usually not expressed. In addition, the aphthous form is not contagious.
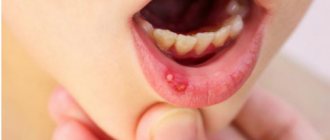
- Herpetic stomatitis is an infectious pathology of the oral cavity that develops due to invasion of the herpes virus. The disease is characterized by the appearance of small, painful, fluid-filled ulcers in the mouth. Foci of infection may appear on the outer surface of the lips. A yellow crust usually forms around the ulcer. Within 5-7 days, the source of infection disappears, however, the herpetic form of the disease is characterized by a relapsing course.
- Candidal stomatitis is an infectious lesion of the oral cavity as a result of invasion of the Candida fungus. This form is usually diagnosed in children and elderly patients. Chronic course is also characteristic.
- Allergic stomatitis is a lesion of the oral mucosa as a result of sensitization of the immune system. Additional symptoms include facial redness, neck swelling, and itching.
- Aphthous stomatitis is the most benign form. This pathology occurs rarely and goes away on its own without the risk of developing a chronic form of the course. Fungal and viral forms of stomatitis, on the contrary, are quite dangerous.
Herpetic stomatitis in children
Causes
This is an infectious stomatitis that occurs under the influence of the herpes virus. There are acute and chronic recurrent herpetic stomatitis. Acute herpetic stomatitis occurs when a child is first infected and occurs most often between the ages of 6 months and 3 years. In 100% of cases, the child gets the infection from parents and other close people (when they lick the child’s spoon and continue to feed him further, lick the pacifier or drink from the same cup). At this age, the child no longer has the antibodies that he gets from his mother’s milk, and has not yet developed his own. Therefore, when a virus enters the body, a disease inevitably begins. In its acute form, such an infection manifests itself in only 10% of children, and all the rest tolerate the primary infection quite easily.
Chronic recurrent stomatitis is due to the fact that the herpes virus, once entering the body, settles there forever and under favorable conditions (the above-mentioned decrease in immunity) can provoke repeated rashes.
The symptoms of acute and chronic herpetic stomatitis are different. In both forms, there are general phenomena (in the body as a whole) and a specific picture in the oral cavity.
Symptoms
Acute herpetic stomatitis
- General deterioration in health. Acute herpetic stomatitis is characterized by weakness, headache, pain in joints and muscles, malaise - general symptoms of intoxication caused by viral activity. The temperature is usually raised to 37 -41 degrees in the first or second day. The lymph nodes (especially the submandibular ones) enlarge and become painful.
In the oral cavity there are:
- swelling;
- redness of the mucous membrane;
- soreness of the mucous membrane in the cheeks, lips, tongue, palatine arches;
- small (the size of a millet grain) bubbles, usually collected in groups filled with a clear liquid; over time, the liquid becomes cloudy, and after 2-3 days the bubbles burst, and a bright red erosion forms in their place. Even later, the surface of the erosion becomes covered with a fibrinous coating (whitish or yellowish). These white spots are surrounded by a red corolla.
- Redness and swelling of the gum edge around the teeth and redness of the interdental papillae are often observed (clinic of gingivitis).
Along with rashes in the mouth, rashes are often observed at the border of the red border of the lips and skin or at the border of the nasal mucosa and skin.
Chronic herpetic stomatitis
All symptoms in the oral cavity repeat the picture of acute herpetic stomatitis, but the general condition, as a rule, does not suffer.
Factors that provoke exacerbations of chronic herpetic stomatitis:
- acute respiratory infections, acute respiratory viral infections, hypothermia;
- avitaminosis;
- allergy;
- stress;
- taking immunosuppressive drugs;
- exacerbation of chronic tonsillitis, sinusitis and other diseases;
- trauma to the oral mucosa;
- foci of infection in the oral cavity (carious teeth, hard and soft dental plaque, gingivitis);
- breathing through the mouth (due to this, drying out of the mucous membrane occurs, which provokes a decrease in local immunity, as well as the formation of cracks on the lips).
Treatment of herpetic stomatitis in a child
Be sure to consult a dentist for an accurate diagnosis. If it is not possible to see a doctor on the first day, you can start treatment, but a visit to the doctor as soon as possible is required.
Antiviral therapy (to combat the pathogen)
- Acyclovir (tablets) or Viferon (gel, suppositories) - depending on the age of the child. Suppositories are more suitable for infants and children up to one year old; older children can be given tablets or treated with gel.
- For rashes that are observed only on the skin, antiviral ointments are used (acyclovir, Viferon, Zovirax and others).
Antiviral drugs are taken according to the regimen specified in the instructions. The sooner you start taking the drug, the more active it will be against the virus. These drugs are taken on days 1-4 of the disease.
Antiseptic treatment (prevention of complications)
- Miramistin (rinse aid) is used directly as a rinse. For young children who cannot yet rinse their mouths themselves, wiping with a gauze swab dipped in a solution of the drug is used. Other antiseptics are either not used at all (since they are not effective against viruses), or are used in combination with miramistin (alternately). You can take chlorhexidine, givalex, rotokan, chlorophyllipt, but all this is only in combination with miramistin.
Keratoplasty (drugs to stimulate mucosal healing)
- solutions of vitamins A and E (you can buy an oil solution at the pharmacy). Applications are made after rinsing with an antiseptic (the drug is applied to a gauze turunda and the wound surface is lubricated).
- rosehip or sea buckthorn oil. Also in the form of applications.
- solcoseryl (after rinsing, apply a thin layer of gel using an ear stick or a clean finger).
One of these drugs to choose from.
Symptomatic treatment
- If soreness of the mucous membrane interferes with eating and hygiene - Dentol or its analogues (drugs used in children during teething) - lubricate the surface of erosions before eating or brushing teeth.
- If the temperature is above 38 degrees - paracetamol, nurofen, ibuprofen, mefenamic acid or any other antipyretics (according to the instructions).
- drinking plenty of fluids to reduce symptoms of intoxication;
- diet excluding spicy, salty, sour, hard foods, allergens (citrus fruits, chocolate, honey);
- Immunostimulants: imunal, amiksin, imudon and others - as prescribed by a doctor.
Causes
Stomatitis can have different etiologies
Doctors are not always able to identify the cause of stomatitis. The inflammatory form of the disease can occur suddenly against the background of complete clinical well-being. It is assumed that the mucous membrane can be damaged under the influence of a variety of negative factors.
Main reasons:
- Minor trauma to the oral mucosa as a result of careless brushing of teeth, an accidental bite, or damage during eating.
- Negative effects of substances contained in toothpastes and mouthwashes. For example, sodium lauryl sulfate can cause an inflammatory process in the mucous membrane.
- Sensitivity to certain foods. As a rule, these are chocolate, coffee, fruits, eggs, nuts, cheese, spicy and sour foods.
- Vitamin B12 deficiency in the diet.
- Insufficient intake of zinc, folic acid and iron from food.
- Allergic reaction.
- Hormonal changes during puberty and the menstrual cycle.
- Chronic stress.
- Entry of pathogenic bacteria, viruses or fungi into the oral cavity.
- Pathologies of immunity.
It is also necessary to take into account the influence of risk factors, the presence of which increases the likelihood of developing the disease. The main risk factors for stomatitis include:
- Inflammatory diseases of the digestive organs. This could be celiac disease, Crohn's disease or ulcerative colitis.
- Gastroesophageal reflux. The contents of the stomach can even enter the oral cavity.
- Behçet's disease is a rare disorder that causes inflammation throughout the body, including the mouth.
- HIV and AIDS.
- Childhood.
- Family history of inflammatory and infectious diseases of the mouth.
Often, stomatitis appears against the background of other inflammatory pathologies of the digestive organs.
Symptoms and signs
With fungal stomatitis, a white coating appears
The symptomatic picture depends on the type of stomatitis. Infectious and inflammatory forms of the disease may have different symptoms.
Main manifestations:
- Painful sensations. The pain may worsen while eating because the skin under the ulcer is very sensitive.
- The appearance of red spots in the mouth.
- Swelling and redness around the ulcer.
- Burning sensation in the mouth.
- Weakness.
- High body temperature.
The most aggressive symptoms are characteristic of candidiasis and herpetic stomatitis.
Diagnostic methods
Dentists, pediatricians and pediatric infectious disease specialists treat inflammatory diseases of the mouth in children. During the appointment, the doctor will examine your complaints, review your medical history to identify risk factors, and conduct a physical examination.
As a rule, a general and instrumental examination of the mouth is sufficient to make a preliminary diagnosis, since different forms of stomatitis manifest themselves as peculiar ulcers. Additional research may be required to clarify the nature of the disease.
Treatment and prevention
Stomatitis affects the general condition of the baby
Therapy should be aimed at the root cause of oral ulcers. Typically, all forms of inflammatory stomatitis resolve on their own within 7-10 days.
Treatment may be required if infection develops or inflammation progresses unfavorably. Therapy is also sometimes required to prevent relapses of the pathology.
The most effective treatment methods:
- Mouth rinse. Oral antiseptics and products containing dexamethasone or lidocaine can be used as a rinse. This method of treatment removes pathogenic microorganisms from the oral cavity, as well as reduces pain and inflammation.
- Pastes, creams and gels for treating the oral cavity. The active ingredients in such products help reduce pain and speed up recovery. Your doctor may recommend medications that contain benzocaine, fluocinonide, or hydrogen peroxide. Before prescribing such drugs, it is necessary to determine the etiology of the disease.
- Oral steroid drugs for severe stomatitis. Usually prescribed if the disease does not respond to other drug treatments.
- Chemical cauterization of ulcers using silver nitrate and other reagents. Helps speed up healing and relieve symptoms.
- Antiallergic drugs with a positive sensitization test.
- Antibiotics, antiviral and antifungal agents.
- Nutritional supplements containing folic acid, B vitamins and zinc.
The listed remedies can only be prescribed by a doctor after a thorough diagnosis. Independent drug treatment is fraught with the development of dangerous complications.
Prevention methods include:
- Avoidance of foods that irritate the oral mucosa.
- Child nutrition appropriate for his age group.
- Maintain careful oral hygiene.
- Rinsing your mouth with special solutions.
- Timely treatment of inflammatory and infectious diseases.
Such methods are also important for preventing recurrences of stomatitis.
Chronic aphthous stomatitis
Causes
Aphthous stomatitis is caused by staphylococcus, a microorganism that is found in large quantities in dental plaque and lives in carious cavities. Every person has this microbe and usually does not manifest itself in any way, but against the background of immune disorders. Often aphthous stomatitis can develop against the background of allergies, gastrointestinal diseases or injuries to the oral mucosa. Another factor in the development of the disease is dirty hands. This disease is often associated with children putting unwashed toys into their mouths, thereby increasing the total number and variety of microbes in the mouth.
Symptoms
Most often, manifestations of chronic aphthous stomatitis occur on the lips, transitional fold, gums, under the tongue and on the tongue - in places where the mucous membrane can be injured by teeth or spicy food.
- Minor change in general health. Characterized by enlargement of the submandibular lymph nodes, fever and weakness.
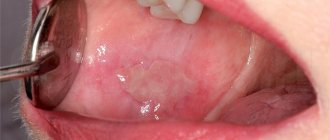
- On an externally unchanged mucosa, aphtha appears - a spot 5-10 mm in size, slightly rising above the surface of the mucosa, covered with a whitish film tightly fused to the mucosa and surrounded by a bright red rim. Aphthae are very painful when touched. Most often there are one or two aphthae, less often – several.
Must remember! It is necessary to accurately determine the type of stomatitis: herpetic or aphthous. With herpetic stomatitis, there are many small blisters that turn into erosions and sometimes merge with each other, and rashes on the lips are possible. With aphthous rashes, larger, single rashes occur only in the mouth. If you have stomatitis, you should definitely consult a dentist to determine the type of stomatitis and choose the right treatment tactics.
Treatment
Elimination of the factor that caused the disease:
- exclude all allergens (citrus fruits, chocolate, brightly colored foods...);
- if you are taking medications that can cause allergies, then you also need to take this into account (tell your doctor what you are taking and for how long);
- exclude rough, spicy, salty, sour foods;
- if stomatitis is caused by allergies, antihistamines (suprastin, loratadine) are prescribed;
- If the aphthae is due to injuries from sharp edges of a tooth or filling, it is necessary to put the tooth in order.
- in the first 3-4 days, treatment of aphthae is carried out exclusively with antiseptics (rinses, gels). You can use chlorhexidine, rotokan, miramistin, givalex, stomatidine, listerine, chamomile and calendula decoctions - you can take any of these drugs (or any other analogue). Use according to the instructions (there are preparations in ready-made form, and there are those that need to be diluted). Rinse (or wipe the mucous membrane in small children) 3-4 times a day.
- after 3-4 days, epithelializing agents are added: solutions of vitamins A and E, rosehip or sea buckthorn oil, solcoseryl.
- If relapses occur frequently, you should pay attention to your general health. In some cases, only joint treatment with an immunologist, gastroenterologist, endocrinologist and other specialized specialists can help cope with the disease.
Must remember! Aphthous stomatitis is, first of all, a microbial lesion. Oral hygiene, adherence to personal hygiene rules, as well as timely treatment of caries, caries complications, and removal of tartar in many cases are sufficient to avoid aphthous stomatitis.