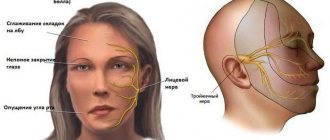
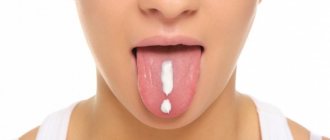
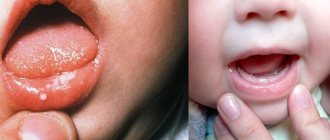
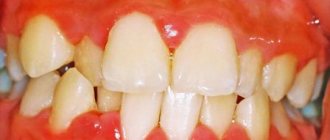
What is stomatitis?
Stomatitis is an inflammation of the oral mucosa. According to statistics, about 20% of the population of our planet faces it. In adults and children, it can take the form of an independent disease or act as a symptom indicating pathologies of the body. In both cases, treatment is carried out comprehensively and under the supervision of a doctor.
What does the disease look like?
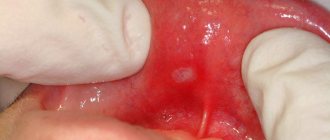
Stomatitis is not difficult to recognize. The initial stage of the disease is characterized by the appearance of mild swelling of the oral mucosa. It becomes redder, drier and shiny. A plaque may appear on its surface, and at the site of future lesions the patient feels an unpleasant itching or burning sensation.
As the disease develops, small ulcers and wounds appear on the mucous membrane - painful oval or round lesions. Their location may be the inside of the lips, cheeks, palate, tonsils, or mucous membrane under the tongue. Their appearance can be seen in the photo at the end of our article.
Treatment of candidal stomatitis
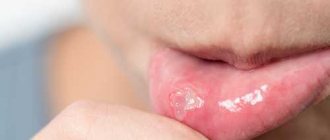
A type of stomatitis that is caused by a special type of fungus – Candida albicans. Very often, candidal stomatitis begins with glossitis, which is why its second name is stomatitis on the tongue. Treatment in this case requires fairly prompt treatment, since in adults it is quite painful and is accompanied by a burning sensation in the mucous membrane and sore throat. On the inner surface of the lips and cheeks, as well as on the tongue, characteristic foci of inflammation appear, covered with a white cheesy coating.
Treatment methods
- Treatment of common diseases (if detected).
- Antimicrobial therapy.
- Preventive rinses.
Causes of stomatitis
The mechanism of stomatitis is not yet fully understood. But scientists are inclined to believe that the root cause of its development is the reaction of the human immune system to various irritants. At some point, the immune system ceases to recognize the potential threat of internal and external factors, which causes its atypical reaction, as a result of which “aggressive behavior” of lymphocytes is observed. The attack of lymphocytes against irritant molecules leads to lesions of the oral mucosa.
A variety of factors can provoke an atypical reaction of the immune system. The most likely of them are the following irritants:
- Pathogenic microorganisms that live in the mouth.
- Improper oral hygiene.
- Various damage to the mucous membrane, for example, burns from eating too hot food or mechanical injuries from seeds, nuts, crackers and other hard foods.
- General dehydration due to high fever, blood loss, vomiting, diarrhea, or thirst.
- Poor quality treatment of teeth and gums.
- An allergic reaction to dental structures in the mouth - braces, implants, crowns, bridges, etc.
- Long-term use of medications.
- A diet depleted of beneficial vitamins and elements.
- Smoking.
- Malignant formations of the oral cavity, respiratory organs or undergoing a course of chemotherapy.
- Hormonal imbalances in the body, for example in pregnant women or children during puberty.
- The presence of chronic diseases or allergies.
- Severe stress.
Interesting to know! Frequent stomatitis in adults can be caused by the use of toothpaste containing sodium lauryl sulfate, a substance added to oral care products to form a thick foam. According to recent studies, it dehydrates the oral mucosa and makes it vulnerable to various types of irritants. Patient observation data confirms the fact that avoiding the use of sodium lauryl sulfate paste can reduce the risk of developing stomatitis in adults by 81%.
Causes of stomatitis
Many factors contribute to the development of stomatitis. One of the common causes of the disease is the action of an irritant . The mucous membrane can be affected by constant mechanical trauma (biting the cheeks and tongue, trauma from tartar, incorrectly made prosthesis or crown) [5]. Injury can be caused by exposure to a thermal or chemical agent, for example, when a mucous membrane is burned by hot food or when an allergy occurs to certain foods (for example, citrus fruits) or medications. The risk group includes smokers, since nicotine also acts as an irritant to the mucous membranes.
Oral hygiene plays a major role in the development of stomatitis. With improper oral care, plaque and tartar accumulate; the microorganisms present in them (staphylococci, streptococci) can cause irritation and inflammation of the oral mucosa. As a result, stomatitis occurs as a protective reaction of the body.
Sometimes inflammation of the mucous membrane occurs in various chronic diseases and pathologies with an unclear etiology (cause). Stomatitis can manifest itself in the oral cavity against the background of diseases of the gastrointestinal tract (with helminthic infection), cardiovascular system, blood diseases (anemia), endocrine disorders (diabetes mellitus). Very often, stomatitis develops during HIV infections and can be one of the diagnostic signs when identifying HIV.
Reason/Example
| Fungal infections | ⠀•⠀Candidiasis |
| Bacterial infections | ⠀•⠀Acute necrotic ulcerative gingivitis ⠀•⠀Syphilis ⠀•⠀Tuberculosis |
| Viral infections | ⠀•⠀Chicken pox ⠀•⠀Herpes simplex virus |
| Physical factors | ⠀•⠀Poorly fitting denture ⠀•⠀Improperly made crown ⠀•⠀Improper bite ⠀•⠀Biting cheeks and lips ⠀•⠀Tartar |
| Medicines | ⠀•⠀Antibiotics ⠀•⠀Barbiturates ⠀•⠀Chemotherapy drugs |
| Allergens | ⠀•⠀Occupational exposure to dyes, acid fumes, heavy metals ⠀•⠀Allergic reaction to food |
| Chronic diseases | ⠀•⠀Diabetes mellitus ⠀•⠀Anemia ⠀•⠀HIV infection |
If you notice similar symptoms, consult your doctor. Do not self-medicate - it is dangerous for your health!
Causes of acute stomatitis
Acute stomatitis occurs most often after damage to the mucous membrane or against the background of a viral disease. Injuries create favorable conditions for the proliferation of pathogenic microorganisms, including the herpes virus. Stomatitis in adults usually has a herpetic form.
Relapses of the inflammatory process usually occur in the cold season, when acute respiratory viral infections, in particular influenza, progress. This coincidence is not accidental. Viral diseases contribute to the appearance of stomatitis in adults and children.
Causes of chronic stomatitis
Chronic stomatitis in the oral cavity regularly worsens. In the summer, a temporary remission is observed. Chronic inflammation is caused by concomitant pathologies of the endocrine system, digestive tract, and diseases of an autoimmune nature. Dental diseases, including caries, periodontal disease, and gingivitis, also contribute to the protracted course of the inflammatory process.
Treatment of stomatitis with folk remedies
Treatment of diseases, especially in the early stages, is possible at home. How is stomatitis in the mouth treated in adults ? Anti-inflammatory and healing folk remedies:
- chamomile with honey;
- burdock root and chicory herb;
- grated raw potatoes (keep in mouth for 5-7 minutes);
- yarrow decoction;
- crushed burdock seeds;
- garlic mixed with curdled milk (or sour cream).
If your body lacks vitamins, you can prepare a vitamin salad.
Burdock leaves, horseradish roots, green onions, sour cream and salt are added to it. Effective treatment of stomatitis at home is possible. The patient must also:
- perform daily oral hygiene;
- follow a diet;
- limit alcohol consumption;
- give up sweets, chips, crackers.
There is a high probability of this disease appearing again. But if you carry out the right treatment, this will not happen.
How to treat stomatitis in children?
Parents who discover ulcers in their child’s mouth are required to contact a pediatric dentist. The following will help prevent the spread of infection:
- limiting contact with other children;
- allocation of separate dishes;
- own personal hygiene items.
The course of therapy consists of taking medications:
- painkillers;
- antiseptic;
- antiviral;
- healing.
How to treat stomatitis in children ? Allowed to process places:
- Oxolinic ointment. Apply 2-3 times daily.
- Acyclovir. The interval between applications is 8 hours.
- Tebrofen gel. No more than 4 times a day.
Pain-relieving ointments can be used. For example, Lidochlor and Kamistad (allowed for 3 months).
Ointments and gels
1. Acyclovir An antiviral drug that has a highly selective effect on herpes viruses. In case of herpes, it prevents the formation of new rash elements, reduces the likelihood of complications, accelerates the formation of crusts, and reduces pain in the acute phase of herpes zoster. The ointment is applied to the affected areas of the skin 4-6 times a day (as early as possible after the onset of infection). Cost: up to 220 rub.
2. Metrogyl denta
A combined antimicrobial drug, the effectiveness of which is due to the presence of two antibacterial components in its composition.
For aphthous stomatitis, the gel is applied to the affected area of the oral mucosa 2 times a day for 7-10 days. The drug is contraindicated in people under 18 years of age. Cost: up to 300 rub.
3. Oxolinic ointment Demonstrates antiviral activity against herpes simplex viruses, herpes zoster, and influenza viruses (mainly type A2). For external use. Non-toxic, non-irritating if the required amount and concentration have been applied and the skin at the application site has not been damaged. Cost: up to 100 rub.
4. Vinilin is a drug that has an antimicrobial, anti-inflammatory, enveloping effect, promotes the cleansing and healing of wounds and ulcers. The antimicrobial effect of the drug inhibits the growth and development of microorganisms. Envelops and regenerates. Vinilin acts as a local anesthetic. Vinylin is usually prescribed by dentists for the treatment of stomatitis, because it has not only antimicrobial, antiviral and antifungal effects, but also healing. A protective film is formed, which protects the wound from irritation upon contact with products, thereby reducing pain. Vinilin does an excellent job of treating stomatitis, but it should be used as prescribed by a dentist. Suitable for any type of stomatitis. Cost: up to 200 rub.
1. Anaferon Lozenges. Immunomodulatory agent. When used prophylactically and therapeutically, it has an antiviral effect. It is used for complex treatment of infections caused by herpes viruses, as well as acute and chronic viral infections. Allergic reactions and increased individual sensitivity to the components of the drug are possible. Contraindications include individual sensitivity to the components of the drug. It is not recommended for use by people with congenital lactose deficiency syndrome. Cost: up to 240 rub.
2. Immunal The drug is in the form of drops for oral administration. Used in cases of decreased immunity, stimulates the immune system in uncomplicated acute infectious diseases. Contraindicated during breastfeeding without prior consultation with a doctor. Cost: up to 340 rub.
3. Givalex Antibacterial and antifungal agent. It has a bacteriostatic and weak bactericidal effect. The drug is in the form of a spray and solution in bottles. It is used as a means for the local treatment of infectious and inflammatory lesions of the oral cavity and pharynx, which are caused by microflora that are sensitive to the action of the drug. It is used to prevent the development of infectious and inflammatory lesions after dental surgery. During pregnancy, use according to strict medical indications. If breastfeeding, use of Givalex should be discontinued. Cost: up to 150 rub.
4. Clotrimazole
Clotrimazole is an antifungal medicine.
Has a wide range of antifungal effects. The active ingredient of the drug is an imidazole antimycotic agent. . This medicine is effective against dermatophytes and yeast fungi. In addition, the drug has an antimicrobial effect. Clotrimazole should not be used if you are hypersensitive (allergic) to clotrimazole, its auxiliary ingredients, or in the first trimester of pregnancy. Cost: up to 360 rub.
5. Ketotifen Ketotifen is produced in tablets and syrup. The main ingredient of the product is ketotifena fumarate. The drug is intended for long-term use. The maximum effect can be achieved only after several weeks of treatment. The average course of therapy can last from 2 to 3 months. Discontinuation of the drug is carried out gradually - from 2 to 4 weeks. Ketotifen is not prescribed to those whose profession involves driving vehicles or potentially dangerous machinery. Cost: up to 100 rub.
6. Tavegil Tavegil in solution for injection is used in the prevention and treatment of pseudoallergic and allergic reactions. Tavegil is not prescribed to patients undergoing treatment with monoamine oxidase inhibitors. In addition, the drug is not prescribed to patients with damage to the lower respiratory system. Cost: up to 200 rub.
Drugs that accelerate the healing of the mucous membrane
1. Vitamin A Has a general strengthening effect, normalizes tissue metabolism, and participates in redox processes. Increases the body's resistance to infection. The drug is taken orally early in the morning or late in the evening, 10-15 minutes after meals, 1 capsule 1 time per day. Long-term daily use can cause intoxication, hypervitaminosis A (headache, nausea, vomiting). Contraindicated during pregnancy and breastfeeding. Cost: up to 100 rub.
2. Sea buckthorn oil Oil preparations always act more gently than aqueous or alcoholic medicinal solutions. This oil can be used if there is no allergy to natural oils. Treatment is carried out by lubricating the areas of erosion a maximum of three times a day. A cotton swab or disk should be dipped in oil and then applied to the mucous membrane. Cost: up to 150 rub.
Anti-inflammatory drugs, antiseptics
Anesthetic (painkiller) drugs dull pain in the mouth for a short time. 1. Hexoral Antiseptic for topical use in ENT practice and dentistry. The drug has a wide spectrum of antibacterial and antifungal effects, in particular against gram-positive bacteria and fungi of the genus Candida. It is prescribed as a symptomatic remedy. The drug is sprayed into the mouth or pharynx, and the affected areas are treated while holding your breath. One injection for 1-2 seconds 2 times a day. The duration of treatment is determined by the doctor. Cost: up to 310 rub.
2. Lidocaine Asept Available in aerosol form. The drug can be used for local anesthesia in dentistry. Apply topically, externally. The dosage varies depending on the doctor's indications. You can also apply it using a cotton swab soaked in it. Contraindications include hypersensitivity to lidocaine. Cost: up to 280 rub.
3. Decathylene Has antibacterial and antifungal effects. Affects microorganisms that cause mixed infections of the mouth and throat. Decathylene does not contain sugar, so it is suitable for people with diabetes. Recommended for aphthous stomatitis. Contraindications – hypersensitivity to any of the substances that are part of the drug. Cost: up to 1300 rub.
Prevention
Prevention helps avoid relapses of stomatitis. First of all, it is worth protecting the mucous membrane from the action of aggressive factors: poor-quality hygiene products, cold or, conversely, scalding food, traumatic dentures and uneven edges of teeth, cigarette smoke, and alcoholic beverages.
Strengthening local immunity plays an important role in preventive measures. The oral mucosa is a protective barrier. If the normal microflora is disrupted, the number of potentially dangerous infectious pathogens increases, they actively multiply and cause a response - an inflammatory process.
To strengthen the immune system, you can use natural factors (hardening with water, sun, air) or natural and artificial immunostimulants.
It is recommended to consume honey in courses, which has antimicrobial activity and functions as a biostimulator. Among medications to strengthen local immunity, it is useful to chew Echinacea tablets and use the drug Imudon.
The presence of bad habits, especially frequent smoking, disrupts the local microflora, irritates the mucous membrane and causes inflammation. Try to gradually reduce the number of cigarettes to give up them painlessly.
Several times a year it is necessary to take courses of multivitamin preparations. Prophylactic treatment usually takes 1-2 months. Pay attention to the quality of your diet. Your daily diet must include vegetables and fruits. Avoid foods that irritate or damage the mucous membrane. Be sure to promptly treat tooth decay and remove tartar at the dentist's office. Carefully choose a specialist who selects the prosthesis and installs it. During the period of adaptation to prosthetics, use the dental gel Cholisal with antimicrobial activity or Metrogyl denta.
Sources:
- https://ProBolezny.ru/stomatit/
- https://stom-info.ru/stomatit/
- https://stomatita.ru/
- https://atvmedia.ru/materials/stomatit-vo-rtu-u-vzroslyh
Symptoms of the disease
Stomatitis can occur at any age. In the early stages, its course is accompanied by swelling, redness and dryness of the oral mucosa. The main sign of the disease is the presence of one or multiple ulcers and their appearance.
- Oval or round ulcer shape.
- Small sizes.
- Smooth edges.
- The presence of a thin grayish or white film in the central part of the ulcer.
- The ulcer is surrounded by a slightly reddish halo.
- The mucosal tissue around the lesion has a normal, healthy appearance.
The slight itching or burning sensation that the patient experienced at the beginning of the disease is replaced by pain. The ulcers hurt when eating, talking and smiling broadly. Any touch to them causes pain, which complicates hygiene measures and leads to bad breath.
On average, the disease lasts from 4 to 14 days. Its clinical picture depends on the individual characteristics of the organism, the form and type of the disease. During this period, in addition to the main signs of pathology, other symptoms of the disease may be observed.
- Increase in temperature - during the first days, until characteristic ulcers appear (in severe forms of stomatitis, the elevated temperature persists throughout the entire illness).
- General malaise and fatigue.
- Chills.
- Headache.
- Lack of appetite (especially in children).
- Enlarged lymph nodes (in rare cases).
Important to remember! Severe inflammation, toothache or high temperature for a long time indicate a severe form of stomatitis or the development of its complications. In this case, immediate medical attention is required, and if necessary, hospitalization of the patient is possible.
How to treat stomatitis?
Any treatment for stomatitis begins with a professional hygienic cleaning procedure, during which tartar and soft plaque are removed. Almost any dental clinic in Moscow provides a similar service. Teeth affected by caries are treated. The mucous membrane is treated with antiseptic rinses. During the day, rinse the mouth with a warm solution of chamomile or calendula decoction. With timely treatment, catarrhal stomatitis disappears in 5–10 days. For ulcerative or aphthous stomatitis, local treatment is combined with general treatment. In addition to professional oral hygiene, antiseptic procedures are carried out in the clinic where stomatitis is treated.
If the presence of herpetic stomatitis is suspected, additional antiviral therapy is carried out. In case of oral candidiasis, treatment is prescribed with antifungal drugs. If the cause of stomatitis is some other disease, for example, the stomach or intestines, then it is necessary to begin to treat the root cause. During the treatment process, you should definitely follow a diet limiting spicy, hot, cold, sour and rough foods. A side effect of taking medications can be a green coating on the tongue.
Can stomatitis go away on its own?
As a rule, mild forms of the disease caused by trauma to the mucous membrane, poor oral hygiene or an allergic reaction of the body can go away on their own. Severe stomatitis caused by infection requires qualified treatment. In both cases, it is better not to wait and not to self-medicate. Because the disease not only causes pain and discomfort, but can also lead to generalization of infection and serious complications.
Consequences and complications of the disease
Possible complications arise when the patient ignores treatment for stomatitis. As a result, mild and severe forms of the disease become chronic. The neglected process turns into an ulcerative-necrotic and then gangrenous form of the disease, as a result of which not only the mucous membrane is damaged, but also the soft tissues of the mouth and jaw bones.
Other serious consequences of untreated stomatitis include the following complications.
- Bleeding gums.
- Scarring of the oral mucosa, disruption of its elasticity and mobility.
- Attachment of a secondary infection.
- Tooth loss.
- Voice changes – hoarseness, hoarseness.
Important to remember! A small ulcer on the oral mucosa is a potential threat to the entire body. Infection from it can spread to other organs and systems, which will disrupt the functions of the heart, liver, kidneys, gastrointestinal tract and respiratory organs.
Allergic stomatitis
They arise as a reaction of the mucous membrane to an allergen. An allergic agent can be toothpastes, mouthwashes, food, medicines, materials for crowns, fillings, etc. Allergies often occur to removable dentures. The mucous membrane is affected precisely at the point of contact with the damaging agent, for example, the hard palate under a removable denture. With allergic stomatitis, the mucous membrane is swollen, red, bubbles appear, which burst with the appearance of painful erosions.
Allergic stomatitis also includes chronic recurrent aphthous stomatitis , it begins with swelling and burning, then a painful aphtha appears, and then a healing period begins. This disease is characterized by constant relapses with a certain frequency.
Folk remedies
For treatment, you can use traditional medicine. The following juices, decoctions, oils and infusions have proven themselves well.
You can gently lubricate the affected areas of the mucous membrane with juices and oils. Solutions and decoctions of herbs are used for regular rinsing of the mouth.
Important! Before using traditional medicine, you should consult a doctor. Only a specialist can determine the advisability of their use without harm to health. The use of folk remedies does not cancel the main therapy, but only complements its effect.
Treatment of bacterial stomatitis
This type of stomatitis is also called prosthetic stomatitis, since it occurs due to unsatisfactory care of the orthopedic structure, when many pathogenic microorganisms accumulate in the area of contact between the prosthesis and soft tissues. After treating foci of inflammation, it is necessary to carry out complete cleaning and antibacterial treatment of the prosthesis or replace it. This type of stomatitis should not be confused with allergic stomatitis, which develops against the background of an allergy to the prosthetic material. In this case, the prosthesis must be changed to a hypoallergenic one.
Treatment methods
- Anti-infective therapy.
- Mouth rinse.
How many days does treatment last?
Correct, competent treatment of stomatitis significantly speeds up the healing process. Depending on the type of disease, it lasts for 3 to 7 days. If after 1 week of treatment the signs of the disease have not disappeared or worsening is observed, then the patient most likely has complications. The following factors may be the probable reasons for its development.
- The patient self-medicated or did not follow the doctor's instructions.
- Decreased immunity.
- The presence of chronic diseases of the body.
- Regular injury or infection of the oral mucosa.
- Undiagnosed allergy.
- Having bad habits - smoking, chewing, etc.
- Depression or frequent stress.
- Improper oral hygiene.
- Uncontrolled use of medications.
- The use of oral hygiene products containing sodium lauryl sulfate.
Returning to the question - can stomatitis go away on its own - it should be noted that a seemingly harmless disease can turn into serious problems for the patient. Therefore, you should remember three “don’ts” - don’t
engage in self-medication,
do not
put off visiting a specialist and
do not
ignore the recommendations of your doctor.
How to understand that stomatitis has passed?
Very simple! A complete cure is indicated by the absence of lesions in the oral mucosa. There are no small ulcers, wounds or plaque on the cheek, palate, lip, tongue or tonsil area. The mucous membrane looks healthy, is well moisturized, does not cause pain and does not create discomfort during eating, talking, smiling and performing hygiene procedures.
Treatment of stomatitis at home
I would like to immediately note that treating stomatitis with folk remedies at home is possible, but you need to understand that in many cases it is impossible to do without a visit to a specialist and the use of antibiotics. Ignoring these points can lead to worsening of the disease and longer rehabilitation. In addition, on the Internet you can find a whole lot of “revolutionary” recipes for stomatitis, so you need to be able to separate the wheat from the chaff and understand which remedies can really help, and which are the fruit of the inflamed imagination of “couch healers”. Below we publish the most common methods of preventing and treating stomatitis with folk remedies, but please note that only an experienced specialist can draw up an optimal treatment plan.
In the case of children, treatment of stomatitis with folk remedies at home is used quite often. This is especially justified as a preventive measure, since the child’s body is more susceptible to the influence of the external environment. The most popular remedies are considered to be all kinds of decoctions, for the production of which chamomile, calendula, burdock, propolis and blackberry leaves are used. A homemade ointment is also used to treat stomatitis, which is made from novocaine, egg white and honey. Be that as it may, if your child shows signs of stomatitis, it is best to immediately take him to a specialist who can make the correct diagnosis and plan treatment.
Types of stomatitis in adults
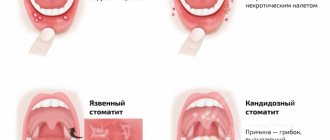
The clinical picture of the disease indicates that stomatitis can be mild or severe, have an acute or chronic course. To facilitate the diagnosis and treatment process, experts have developed the following classification of the disease.
- Allergy is usually a chronic disease that occurs as a result of an allergic reaction of the body to an irritant. In addition to the characteristic ulcers, it may be accompanied by the appearance of white spots, blisters and small hemorrhages on the mucous membrane.
- Herpetic or herpes - the disease occurs due to the entry of the causative agent of the herpes virus into the human body. Stomatitis of this type is characterized by an acute course. Bubbles appear on the surface of the mucous membrane, which open to form erosions and crusts.
- Traumatic (bacterial) – a consequence of mechanical trauma to the oral mucosa and infection entering the wound. As a rule, the disease is mild, with symptoms characteristic of stomatitis.
- Catarrhal and catarrhal-hemorrhagic stomatitis is a mild form of stomatitis, the causes of which are poor oral hygiene, the development of candidiasis, decreased immunity or gastrointestinal pathologies. The disease is accompanied by a typical clinical picture for the disease.
- Candidal (fungal) stomatitis is an acute form of the disease, the so-called thrush, caused by the activity of bacteria of the genus Candida. It is most common in young children, the elderly, and patients who overuse antibiotics. Accompanied by the appearance of a white coating on the mucous membrane, a burning sensation and an unpleasant taste in the mouth.
- Ulcerative is a severe form of the disease that occurs independently or as a result of a complication of the catarrhal course of stomatitis. It occurs acutely, with increased body temperature and enlarged lymph nodes. The resulting ulcers are very painful and can unite and form extensive lesions of the mucous membrane.
- Aphthous stomatitis is a severe form of the disease, occurring acutely or chronically. Accompanied by the appearance of single or multiple gray-white ulcers. The ulcers are surrounded by a red halo and are very painful.
It is important to know! By analyzing the condition of the oral mucosa, the nature of the ulcers and the patient’s complaints, specialists accurately determine the type of stomatitis and make an accurate diagnosis. Thanks to this, treatment of the disease occurs quickly and without complications.
How to get rid of stomatitis?
Stomatitis is perhaps the most common and unpleasant disease of the oral cavity. When an infection enters the body, ulcers form in the mouth. They cause discomfort and can subsequently lead to serious complications. How to treat stomatitis ?
Treatment of any infectious diseases first of all involves going to the doctor. Antibacterial therapy should be carried out under medical supervision. Bacterial disease most often goes away in 1-2 weeks. If the stage is not advanced, it can be treated independently. How to treat stomatitis at home :
- Rinse your mouth with soda solution. Add 1 spoon of soda to a glass of warm water. You can also use boric acid (1 teaspoon per 150 ml of water) or hydrogen peroxide (1 teaspoon per half a glass of water).
- Chamomile decoction. Heals wounds quickly.
- Sea buckthorn oil has an antibacterial effect. You can use antiseptics: chlorhexidine or miramistin.
- Anesthetic dental gels will help relieve severe pain. They should contain lidocaine.
Soda solution can also be used to treat stomatitis in infants .
Wipe the mouth and tongue with moistened gauze. If signs of stomatitis (bacterial) do not disappear, you should consult a doctor.
In case of aphthous form of the disease, you should urgently go to the clinic. How to determine:
- multiple large and deep ulcers;
- grayish coating in the center;
- red rim around the wound.
This type of stomatitis should not be treated at home. It is forbidden to cauterize ulcers with alcohol, iodine, or brilliant green. An advanced disease can lead to suppuration and tissue death.
How to get rid of stomatitis in children?
Basic methods of local therapy:
- Treating the oral cavity with baking soda. For preparation you will need 1 tablespoon per glass of boiled water. Apply 3-6 times a day.
- Rinse with Blue solution. Or 2% boric acid.
- Use of antifungal agents. This includes medicated creams and ointments. For example, Clotrimazole, Pimafucin, Nystatin, Candide.
Symptoms of stomatitis in children and treatment can be determined by a doctor. Treatment is carried out in accordance with the doctor's prescriptions. If the dosage is not followed correctly or the course is interrupted, side effects may occur.
You should not self-medicate, as this can harm the baby.
Only a pediatric dentist will prescribe the correct therapy. He can also advise treating stomatitis in children at home .
Types of stomatitis
Depending on the depth of tissue damage and the cause of inflammation, experts distinguish the following types of stomatitis:
- catarrhal;
- aphthous;
- candida;
- ulcerative;
- herpetic;
- traumatic;
- allergic.
The catarrhal form of stomatitis is the mildest and rarely causes complications. But treatment is still required, mainly local. The most severe course is ulcerative necrotizing stomatitis, which often causes bacterial complications.
The candida type occurs more often in young children.
Each type of disease has its own characteristics, causes of development and symptoms. It is difficult to determine the shape yourself.
Sometimes even specialists do not have enough clinical picture to make an accurate diagnosis. Additional laboratory tests are often required to determine why stomatitis occurs in the mouth and whether it is associated with other diseases.
Which doctor should I contact for stomatitis?
If you notice the first signs of damage to the oral mucosa, you should immediately consult a dentist. After differential diagnosis of the disease and an accurate diagnosis, it is possible to observe it with a general practitioner or other specialized specialist, for example, an allergist.
Do not ignore preventive visits to the dentist.
It is enough to visit a specialist 1 – 2 times a year, which will allow you to promptly identify any dental problem at an early stage of development. This means that its elimination will be quick, easy and without complications.
By clicking the “request a call” button you agree to the personal data processing policy.
Gels and ointments
The use of a variety of creams, gels, and ointments helps reduce pain, prevent the development of complications, relieve inflammation, and speed up the patient’s recovery. They form a protective film on the surface of the mucosa that promotes wound healing.
The effectiveness of ointments such as cholisal, vinylin, kalgel, lidochlor, levomekol has been proven. For the fungal form of the disease, miconase and methyluracil are used. To heal aphthae, sanviritrin and solcoseryl are used.
Below we will tell you about other popular ointments and gels.
Oxolinic ointment
For herpes stomatitis, especially in children, oxolinic ointment is used. It prevents the spread of the disease. The ointment is applied to the inflamed areas of the mucous membrane 3-4 times a day. It is advisable to first rinse your mouth with herbal decoctions or antiseptic solutions.
Metrogil Denta
The modern antiseptic Metrogyl Denta is prescribed for the treatment of aft. The gel is applied with a finger or a cotton swab directly to the surface of the aphthae twice a day. Not used in the treatment of children under six years of age.
Acyclovir (ointment)
The antiviral drug Acyclovir is effective in treating herpes infections. Anti-stomatitis ointment Acyclovir is prescribed for the herpetic form of the disease. Apply to the affected mucous membrane five times a day for a week.
Nystatin ointment
Intended for external use, it is used extremely rarely for the treatment of stomatitis. Nystatin ointment can be prescribed for oral candidiasis if alternative medications are ineffective. Apply a small amount to avoid overdose.
Kamistad gel
An excellent anti-inflammatory and analgesic, Kamistad gel is used in the treatment of all forms of stomatitis. Apply to the affected surface several times a day until complete recovery.
How to distinguish stomatitis from other diseases?
The main sign of stomatitis is the presence of characteristic ulcers, the tissue around which looks healthy. The disease is rarely accompanied by systemic symptoms and, as a rule, recurs from time to time. For a competent specialist, it is not difficult to distinguish stomatitis from other ailments.
For a sore throat
When you have a sore throat, your body temperature always rises. In this case, it is not the ulcers themselves that hurt, but the throat area. Upon visual examination, the tonsils appear swollen, inflamed and red.
For herpes
The problem is that herpetic stomatitis is one of the manifestations of herpes. A viral disease is accompanied by the formation of characteristic blisters that burst and dry out. In the presence of other types of stomatitis, the nature of the ulcers is completely different.
For cancer
Ulcers due to cancer of the oral mucosa do not go away on their own even after treatment. Over time, they increase in size and may bleed and become painful.
From thrush
Candidal stomatitis is thrush caused by the activity of bacteria of the genus Candida. In all other cases, the nature of the disease will be different and can be easily distinguished from thrush by the presence of characteristic ulcers.
For syphilis
When infected with syphilis, a red spot appears on the surface of the mucous membrane. Gradually it thickens, takes the form of a dense nodule and ulcerates - a typical hard chancre is formed, which is completely different from ulcers with stomatitis.
Stomatitis caused by fungi
Candidal stomatitis is a fungal disease caused by fungi of the genus Candida.10 Young children and the elderly are more often affected; people with diabetes and xerostomia (dry mouth), pregnant women and people with weakened immune systems are also at risk. Elderly people wearing removable dentures often get sick.
The main symptom of fungal stomatitis is a burning sensation and the presence of a white, cheesy coating, when removed, a swollen, red mucous membrane appears. The general condition of adults with candidal stomatitis is practically not affected.
Recommendations during treatment
Treatment of stomatitis should be carried out comprehensively - local therapy, taking medications appropriate to the type of disease, and strengthening the immune system. During the treatment period, you must adhere to the following recommendations.
- Compliance with the diet - you need to exclude from the diet spicy, salty, sour, too sweet, smoked, hot, cold and any dishes that are traumatic to the mucous membranes.
- Maintaining oral hygiene . To maintain it, it is necessary to use antiseptic agents that you regularly rinse your mouth with.
- Taking vitamin-mineral complexes that strengthen the body's protective functions.
If the doctor has diagnosed the presence of candidal stomatitis, then you should not drink milk or consume fermented milk products, which activate the activity of pathogenic fungi.
Any medications should be used only as prescribed by a doctor. Especially antibiotics.
It is important to know! It is not recommended to cauterize emerging ulcers with pure alcohol solutions. The only thing that is allowed is treating the lesions with a weak solution of iodine or potassium permanganate.
Answers to popular questions
Which doctor treats stomatitis?
The dentist, if necessary, can refer the patient to other doctors.
Do I need to take antibiotics for stomatitis?
Some forms of stomatitis require the use of antibacterial agents, but in most cases this is not only useless, but even dangerous, since it can lead to dysbacteriosis. Antibiotics should be taken only as prescribed by a doctor in the prescribed dosage.
How long does it take to treat stomatitis?
Depends on the severity and form of the disease. On average 7-10 days.
Is stomatitis contagious?
Not all forms of stomatitis are contagious. Traumatic stomatitis is absolutely not contagious. If stomatitis is caused by viruses, such as herpes or measles, the risk of infection is very high.
Prevention
To avoid the occurrence of stomatitis and its relapses, you should adhere to the following recommendations.
- Maintain oral hygiene.
- Avoid using products containing sodium lauryl sulfate.
- Protect the oral mucosa from injury.
- To treat teeth and gums, contact experienced, qualified specialists.
- Balance your diet with healthy foods.
- Strengthen immunity.
- Be attentive to your physical health and psycho-emotional state - if necessary, seek help from specialized specialists.
And do not forget that herpes stomatitis can be transmitted from person to person - follow the rules of hygiene.
Treatment of aphthous stomatitis
A distinctive feature of this type of stomatitis is the appearance of so-called aphthae on the oral mucosa. These are small round ulcers with redness at the edges, the touch of which causes unpleasant painful sensations. Often occurs as a result of the activity of microorganisms (in particular, staphylococcus). Treating aphthous stomatitis at home is only recommended if it is not caused by a more severe illness. Often aphthous stomatitis occurs with problems with the immune system, liver and gastrointestinal tract.
Treatment methods
- Allergy therapy.
- Antiseptic therapy (treatment of aphthae with anti-inflammatory solutions, gels and ointments).
- Dental treatment and sanitation of the oral cavity (after dental treatment, stomatitis occurs less frequently than in the presence of carious lesions).
- Immunotherapy.
- Diet.
Photo of stomatitis
Author: Elena Grunina Dentist-therapist, endodontist. Work experience more than 9 years. The information is for reference only. Before treatment, consultation with a doctor is necessary.
Tablets and antifungal drugs
When treating advanced forms of the disease, one cannot do without the use of tablets and antifungal drugs. They have a systemic effect on the human body, reduce inflammation, and promote a speedy recovery.
Among the most popular antibiotics are amoxilav, sumamed, flexmoxin solutab. Additionally, the doctor may prescribe anti-inflammatory drugs - imudon, methyluracil, biseptol.
Nystatin
Used in the treatment of candidal stomatitis. Its effectiveness is questionable. The course of treatment with nystatin is quite long. There are alternative modern drugs that help the patient recover faster.
Fluconazole
A strong antimycotic drug that is effective in the treatment of candidiasis. Fluconazole is prescribed 100 mg per day for 7-14 days for all forms of the disease. For recurrent stomatitis, pulse therapy is used - 150 mg once a week.
Lysobacter
Lizobact lozenges are used for stomatitis, sore throat, and tonsillitis. They have local antimicrobial and antiseptic effects. Prescribed for adults and children over three years of age. Take according to instructions.
Streptocide
Quite rarely used in the treatment of stomatitis due to its dubious effectiveness. Pour streptocide, ground into powder, onto a cotton swab, apply to the sore, and hold for 30 minutes. It is advisable not to swallow.
Candide
The antifungal drug Candide prevents the proliferation of fungi. It is prescribed for the treatment of candidal stomatitis. The solution is applied to the affected surface 3-4 times a day until complete recovery.
Prevention of stomatitis
Preventing a disease from occurring is much easier than treating it. Considering that the main risk factors for stomatitis most often are decreased immunity and poor oral hygiene, as well as bad habits, we can name the key points for preventing stomatitis:
- regular teeth cleaning and visits to the dental office,
- taking care of the immune system - avoiding stress, taking multivitamins, eating fruits and vegetables,
- getting rid of bad habits (primarily smoking),
- take care of your health and try to prevent the development of chronic diseases.
When visiting a dentist to install orthodontic structures, dentures, or crowns, you must carefully choose a clinic to avoid allergies or rubbing of the dentures.
Stomatitis and coronavirus
There is a lot of talk now that many people develop stomatitis due to coronavirus. And so the question arises - how are they connected? It is quite obvious that coronavirus infection greatly weakens the body, undermines the immune defense, and leads to various complications. And with a decrease in immunity, as we know, many dormant infections in the body are activated, which lead to stomatitis. Therefore, it is impossible to consider stomatitis as a symptom of Covid. But it is more logical to look at stomatitis as a concomitant disease that occurs in approximately half of those suffering from coronavirus infection.
After coronavirus, stomatitis can also occur as one of the possible complications. Particularly susceptible to this are those patients who did not closely monitor the condition of the oral cavity, rarely visited the dentist, who had advanced caries or problems with the gums (gingivitis, periodontitis), and tartar deposits. In order to avoid contracting stomatitis after Covid, it is important to regularly and thoroughly perform oral hygiene, brush your teeth, and visit the dentist in a timely manner.
Stomatitis rarely occurs after vaccination against coronavirus. Some patients have a more difficult time with vaccination, so a decrease in immunity may result in a recurrence of stomatitis, especially in those who have had it before or in those who are at risk.
Sprays and aerosols
Inhalation with sprays for stomatitis is rarely used. They are indicated if instant results are needed. The medicine is immediately absorbed into the mucous membrane, so relief comes quickly.
Medicines in the form of a spray or aerosol should absolutely not be used in the treatment of children under 6 years of age, as they may inhale the drug.
Below we will introduce you to some fast-acting medications.
Bioparox
The inhalation drug Bioparox is used both for the treatment of diseases of the ENT organs and in dentistry. Has anti-inflammatory and bacteriostatic effects. It contains the polypeptide antibiotic fusafungin. Apply to the surface of the oral cavity 2 times a day.
Tantum Verde spray
The anti-inflammatory pain reliever Tantum Verde is available in the form of a spray and rinse solution. The only spray that is approved for use by infants. Used in the treatment of respiratory diseases. In dentistry it is prescribed to quickly relieve the symptoms of stomatitis.
Ingalipt
The combined drug has a disinfecting and anti-inflammatory effect. Effective in various forms of the disease. Ingalipt is applied to the affected areas of the mucous membrane 3-4 times a day. The course of treatment is 5-7 days. Before use, it is recommended to rinse your mouth with boiled water.
Ambassador
Effective in the treatment of ulcerative, aphthous, catarrhal stomatitis. Proposol contains propolis, glycerin and ethyl alcohol, so it has antimicrobial and anti-inflammatory effects. Spray in the mouth 2-3 times a day for a week.
We have told you different ways to cure stomatitis at home. It is advisable to consult a doctor about prescribing certain medications.
You should not take a large number of different medications at the same time. It is enough to choose one or two of the most effective products plus a variety of rinses.
What consequences might you face?
Most often, the disease goes away within two weeks, but with complicated pathology, the disease can lead to dangerous consequences .
The most common are:
- loss of teeth;
- bleeding gums;
- damage to the hard/soft palate;
- ulcers;
- periodontal disease;
- risk of damage to other areas of the mucous membrane (eyes, genitals);
- general intoxication;
- hoarse speech;
- laryngitis;
- fungus.
Remember! The most dangerous consequence of the disease is fungus. When it enters the bloodstream, it spreads harmful microorganisms throughout the body.
What does stomatitis look like in the mouth?
Initially, during stomatitis, the soft tissues located in the oral cavity swell greatly and swell. The mucous membrane may itch and hurt when fingers press on it. In those places where the rash occurs, the skin may become pale or red. Sometimes tissue hyperemia is noted, so the patient may claim that the mouth is on fire. Later, rashes are observed. Their shade, shape, type depends on stomatitis and its type.
Usually the rashes look like oval or round lesions on the skin, there may be plaque, but the disease is always accompanied by pain. There may be a different number of formations.
Symptoms
It is worth knowing about other manifestations of stomatitis. The most common signs include:
- Initially, the symptoms may resemble a standard cold (headache, joints, muscles, bones hurt, temperature may rise, sometimes a runny nose, pain in the throat);
- the lymph nodes become enlarged, it’s even painful to touch them;
- due to pain, a person or child may completely refuse to eat, and apathy is observed;
- stomatitis can be caused by staphylococcus or streptococcus, and the disease appears against the background of a sore throat. Then the person has purulent discharge, thick saliva containing mucus, and an unpleasant odor from the mouth;
- The soft tissues of the cheeks and lips are damaged, tartar appears, cracks, and the mucous membrane becomes very dry. This is noted in those patients who smoke;
- in the case of a fungal infection as a pathogen, the surface of the mucous membrane is usually covered with a cheesy white coating;
- in the case of an advanced form of stomatitis, rashes appear even on the skin;
- if the disease was provoked by viral agents, then ulcerative and aphthous lesions may also affect other parts.
Types and forms of stomatitis
What types of stomatitis are there? Depending on what is taken as the basis for the classification, various forms and varieties of this disease can be distinguished. For example, according to the degree of damage to the mucous membrane, a distinction is made between catarrhal (superficial) stomatitis and ulcerative stomatitis.
According to the causes of occurrence, traumatic stomatitis, bacterial, candida, viral, prosthetic, drug, allergic and radiation are distinguished. The nature of the course of the disease and the presence of relapses make it possible to determine such forms of stomatitis as acute and chronic stomatitis.
To accurately determine the type of stomatitis in a particular case, it is necessary not only to carefully examine the oral cavity, but also to conduct tests for the presence of certain pathogens, and also take into account the presence of allergic reactions in the patient, chronic diseases (such as diabetes or gastritis) , pathologies of the immune system.
Chronic
Chronic stomatitis usually occurs as a continuation of advanced acute stomatitis and is characterized by a long course with periodic remissions and exacerbations. By origin, this is most often viral (herpetic) stomatitis. After treatment, the virus remains in the body and when the immune system is weakened again (due to stress, illness or other reason), it is activated and leads to relapse of stomatitis.
Chronic recurrent stomatitis can be not only viral in nature, but also bacterial, allergic, and candidiasis. The causative agents of many diseases are constantly present in the body, or easily enter it from the external environment. And if stomatitis was caused by an allergy to some substance or exposure, then it is very likely that with each contact with this allergen the stomatitis will return again.
Treatment of chronic stomatitis always includes the use of specific therapy aimed at suppressing the pathogen: antibacterial, antiviral, antifungal. It is also necessary to eliminate foci of infection (for example, carious cavities) and complete sanitation of the oral cavity with professional hygiene.
Bacterial
Bacterial stomatitis is caused by pathogenic microorganisms (for example, streptococci or staphylococci) that enter the oral cavity or are already in it (for example, in carious cavities, in the thickness of tartar) and infect the mucous membrane. This is facilitated by injury to the mucous membrane with sharp edges of teeth, rubbing dentures, or other objects.
Treatment of bacterial stomatitis involves the use of antiseptic and antibacterial agents. If the cause of stomatitis is a denture, then it should be cleaned with special means (for example, in an ultrasonic bath), or replaced with a more comfortable one.
Angular
Angular stomatitis is associated with the appearance of cracks in the corners of the mouth (“jams”). The main causes of this disease are lack of vitamins and bacterial (or fungal) infection. This type of stomatitis is characterized by damage to the outer surface of the lips.
Treatment for angular stomatitis depends on the type of infection. For fungal infections, fungicidal ointments and preparations are used. The streptococcal variety requires the use of antibacterial agents. Treatment is complemented by taking vitamins, eliminating their deficiency and raising the level of immune defense.
Viral
Viral stomatitis is caused by infection of the body with a virus. Most often (in about 80% of cases) this is the herpes virus. But besides it, stomatitis can be caused by almost any virus - chickenpox, measles, influenza, adenoviruses or rotaviruses. Typically, the onset of the disease is typical for a viral infection of this type - it may be fever, chills, runny nose, cough, or swollen lymph nodes. But after 1-3 days, characteristic symptoms of viral stomatitis appear: blisters form in the mouth, which later turn into ulcers, swelling of the gums, bleeding, and putrid breath may occur.
Viral stomatitis can be considered a complication of the underlying viral infection. Its causes (in addition to the virus itself) are reduced immunity and poor oral hygiene - the presence of untreated caries, periodontal disease, gingivitis.
Treatment of viral stomatitis involves first of all treating the underlying disease. In addition, the affected areas of the mucosa can be treated with local antiseptic drugs, anti-inflammatory and wound healing agents. Often in such cases, antiviral ointments or gels are prescribed, and vitamins, immunomodulators, and adaptogens are prescribed to maintain and strengthen the immune system.
Allergic
Allergic stomatitis is caused by exposure to allergens. In addition to the typical allergens that are well known to us, such as animal fur, pollen, foods such as honey, citrus fruits, etc., allergies can be caused by some medications, dental products and orthodontic structures (for example, acrylic dentures).
It often happens that an incorrectly manufactured prosthesis (for example, with a violation of the proportions of the material components) causes an allergic reaction and, as a result, stomatitis. When replacing the prosthesis with a correctly made one (without excess monomer in the composition), the allergy disappears. Symptoms of allergic stomatitis are redness of the mucous membrane (and with prosthetic stomatitis, this can be not only the areas under the prosthesis, but all parts of the tongue, cheeks, etc., in contact with the prosthesis), swelling, itching, and subsequently small blisters appear, often turning into sores.
When treating allergic stomatitis, it is important first of all to determine the cause of the allergy and remove contact with the allergen (eliminate foods that cause allergies, or replace the denture if this is the cause), and take antihistamines. The rest of the treatment involves the use of local antiseptic, anti-inflammatory and analgesic agents.
Herpetic
Herpetic stomatitis is one of the contagious forms of stomatitis. Moreover, contagiousness persists even for 2 weeks after recovery. In most cases, the herpes virus never completely leaves the infected body. It is in a dormant, inactive form, but can be activated when immunity decreases - due to stress, lack of vitamins, due to a severe respiratory disease. Therefore, herpetic (cold sore) stomatitis is often chronic.
An adult very often does not have a strong reaction to the effects of herpes and damage to the mucous membrane. In children, acute herpetic stomatitis can be accompanied by an increase in temperature, general intoxication; when the bubbles merge, burst and form erosion, the child may feel severe pain, which interferes with eating, drinking, and talking. Most often, rashes appear on the palate, tongue, and inner surface of the cheeks. But often they also affect the lips and gums. The danger of this type of stomatitis is that it can turn into gingivitis, so it must be treated.
Treatment of herpetic stomatitis always involves suppressing the herpes virus. Antiseptics (chlorhexidine) and even many antiviral drugs do not affect the herpes virus. Moreover, antibiotics have no effect on him. Special medications have been developed against herpes - acyclovir, valacyclovir, famciclovir. They should be taken only as prescribed by a doctor, in case of severe herpetic stomatitis.
Among the local antiseptics, you can use Miramistin (effective against both types of herpes viruses) and Hexoral (active only against HSV-1). Anti-inflammatory drugs (cholisal) and wound-healing agents (solcoseryl, actovegin, sea buckthorn and rosehip oil, vitamins A and E) perform well.
Candida
Candidal stomatitis often occurs in children under 3 years of age and is therefore often called childhood thrush. This disease is caused by the fungus Candida. It is distinguished by a characteristic white cheesy coating, which is practically impossible to remove mechanically. When trying to remove it, the patient experiences pain, and under the plaque a bleeding, swollen surface of the mucous membrane is found. At the onset of the disease, a person may feel dry mouth, a burning sensation, and white dots appear that merge to form a continuous plaque.
The decision on how to treat candidal stomatitis should be made by a doctor, especially when it comes to a child. For adults, antifungals and topical medications (such as candida) are almost always prescribed. Treatment of candidal stomatitis in children is often limited to the use of vitamins and immune-strengthening agents. To eliminate symptoms, use alkaline rinses and lubricate the mouth with iodine. Antifungal drugs are used only in cases of severe candidomycosis stomatitis.
Ulcerative
Ulcerative stomatitis is a more severe form of the disease than catarrhal stomatitis. Its peculiarity is that the lesion covers the entire thickness of the mucosa, in contrast to the catarrhal form, where it affects only the superficial layers. Deep damage to the oral mucosa causes great suffering to the patient, and after the ulcers heal, scars often remain. Treatment for ulcerative stomatitis depends on the cause of the disease. If an infection is present, antibacterial, antiviral or antifungal therapy is carried out, as well as a course of restoratives and vitamins. Treatment is carried out with means for topical use - antiseptic drugs (furacilin, chlorhexidine, miramistin), herbal decoctions, healing agents. If the cause is traumatic damage to the mucosa, dental procedures are indicated: removal of decayed teeth, treatment of caries, professional oral hygiene.
Vesicular
Vesicular stomatitis is most often enteroviral. It is usually transmitted from animals (or from people who are carriers of the virus) - by airborne droplets, contact and fecal-oral routes. Children most often suffer from it. One of the characteristic symptoms of this disease is a rash on the palms and soles (sometimes also on the face around the mouth, on the buttocks and genitals) - this is vesicular stomatitis with exanthema.
Watery rashes are quite painful and cause itching, which causes severe discomfort to the child, often leads to refusal to eat, and disrupts sleep. With proper timely treatment, the disease goes away without a trace, leaving lasting lifelong immunity. Unfortunately, there are several types of Coxsackie virus, so a person who has had vesicular stomatitis can become infected again with a different type of virus.
Treatment is mainly symptomatic and includes isolating the patient (to avoid infecting other people), taking painkillers, treating rashes with local antiseptics, using applications and rinses, taking vitamin complexes, and in some cases, antiviral and antihistamine drugs.
Aphthous
Aphthous stomatitis is characterized by the formation of aphthous stomatitis on the oral mucosa - one (less often two or three) round ulcers up to 1 cm in size, surrounded by a bright red border and covered with a gray-yellow coating. Touching them is very painful. Itching or burning is often felt before ulcerations appear. Other symptoms rarely appear - slight fever, weakness.
The cause of aphthous stomatitis is reduced immunity, the presence of foci of infection (chronic tonsillitis, pharyngitis, etc.), gastrointestinal diseases, allergic reactions (including to sodium lauryl sulfate contained in some toothpastes), trauma to the mucous membrane (biting), increased concentration of nitrates in food or drink.
If the situation of decreased immunity, exposure to infections or allergens is repeated, the disease may recur, taking on the character of recurrent aphthous stomatitis. With a mild course of the disease, there are no more than 2-3 relapses per year. More frequent attacks indicate a severe form of the disease.
Treatment of aphthous stomatitis involves eliminating contact with allergens, incl. Avoid toothpaste with sodium lauryl sulfate and avoid allergenic and acidic foods. Antihistamines are also often prescribed.
When deciding how to treat aphthous stomatitis, the doctor must conduct a thorough diagnosis and establish the cause of the disease. In accordance with this, a selection of antiseptic drugs (for example, miramistin or chlorhexidine), anti-inflammatory gels (for example, cholisal) and wound healing agents (solcoseryl) is made.
The severe course of chronic aphthous stomatitis often involves the use of more serious medications and methods: laser treatment, immunomodulators, glucocorticoids, but such drugs should be prescribed exclusively by the attending physician.