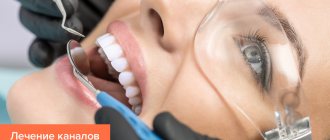
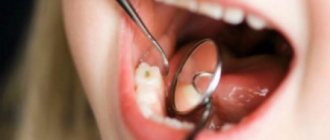
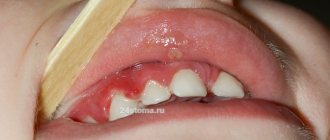
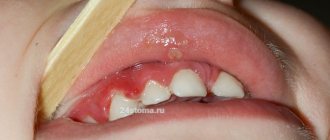
The inflammatory process of the periodontal soft tissues that occurs during complicated or improper teething is called pericoronitis. Inflammation during teething can occur in both adults and children, regardless of the location of the problem tooth, but most often pericoronitis of the wisdom tooth develops (it is also often called the “eight” or third molar).
Causes of inflammation and swollen gums during teething
The main prerequisites for the development of pericoronitis are:
- Mechanical injuries to the gingival tissue over the tooth germs due to hard foods, too hard toothbrushes, as well as due to other damaging factors.
- Long-term or difficult teething.
- Favorable conditions in the mouth for the accumulation of bacterial plaque and food particles under the gingival margin (insufficient hygiene, peculiarities of microflora in the oral cavity).
Swollen gums during teething are easily susceptible to traumatic influences, which leads to the development of inflammation. In this case, teething itself can be difficult for the following objective reasons:
- Dense bone tissue in the “eight” zone; bone compaction is most often formed because there are no milk teeth in this zone.
- There is not enough space for the “eight” in the dentition.
- Thickening of the gums and periosteum in the posterior part of the jaw is usually explained by the characteristics of embryogenesis.
Even one of these factors can cause the disease.
Causes of periostitis:
• of thorough oral care Small children do not yet know how to properly take care of their teeth, so plaque and food debris accumulate in the gum pockets, which can cause inflammation;
• injury to the gums . Children, especially toddlers, love to put almost everything in their mouths. Foreign objects can not only injure the gums, but also introduce harmful microbes into the wounds;
• to caries and its complications . Baby teeth are more vulnerable, so any defect can cause infection;
• angina , tonsillitis . _
Features and risk factors
During difficult and prolonged eruption, the tooth germ practically does not change its position, and a significant part of its chewing surface is covered with a flap of gingival or mucoperiosteal tissue, the so-called “hood”. The flap covering the tooth germ forms a kind of pocket in which food debris and bacterial plaque accumulate. A moist nutrient medium creates optimal conditions for the intensive reproduction of pathogenic microorganisms, which, in turn, actively secrete waste products that are toxic to our body. This provokes the development of an infectious-inflammatory process in the tissues surrounding the problematic tooth germ.
Most often, inflammation of the gums occurs when a wisdom tooth erupts in the lower jaw, which is due to the anatomical structure of the jaw and the lack of space for third molars. In modern people, the jaw arch is approximately 1-1.2 cm smaller than in our distant ancestors, but the size of the teeth has remained the same. This is why the “eights” are cut much later, when the body as a whole and the dental system in particular have already formed - and because of this, it is difficult for the new tooth to find the “right” place on the dental arch.
Since wisdom tooth pericoronitis is the most common type of disease, people over the age of 18 are primarily at risk (usually “eights” are cut at the age of 20-25, but for some this process can take up to 30 years) . As for pericoronitis in children, it usually occurs against the background of insufficient oral hygiene in a child or with infectious diseases of the oral cavity (caries, gingivitis, stomatitis), which complicate teething in children and require treatment. Accumulations of plaque and hard dental deposits significantly increase the risk of developing the disease, so timely and regular removal of tartar can serve as a good preventative method.
Pericoronitis, symptoms and types
With pericoronitis, the symptoms largely depend on the form of the disease - acute or chronic. Acute pericoronitis is characterized by:
- Aching intense pain in the area of the cutting tooth, the pain intensifies under the influence of food and mechanical irritants (hygienic procedures, chewing, touching, etc.).
- Difficulty chewing food, complicated swallowing. A few days after the onset of inflammation, it becomes difficult to open the mouth and severe pain appears.
- Swelling and hyperemia of the mucous membrane.
- Enlargement of regional lymph nodes, sometimes the lymph nodes become painful when touched.
- Externally noticeable swelling of the cheeks a few days after the onset of the inflammatory process.
- General deterioration in health - weakness, lethargy, prolonged low-grade fever (increased temperature to 37-37.5 degrees).
- Bad breath, which is caused by the decomposition of food particles and the active activity of microorganisms in the “hood” space.
Acute pericoronitis can occur in a serous (catarrhal) or purulent form: in the first case, the signs of inflammation are more pronounced, the pain is more intense, and there is no purulent discharge. In the second case, purulent exudate flows freely from the inflammatory focus, due to which tissue tension is somewhat reduced and the symptoms are less pronounced. A person may feel like their condition is gradually improving, when in fact the infection is simply spreading to other tissues in the mouth.
If treatment for acute pericoronaritis was not carried out or was carried out at home, the disease gradually becomes chronic: the severity of symptoms decreases, while exacerbations of pain and discharge of pus into the oral cavity are periodically observed. In this case, there is a high risk of developing severe complications.
Complications of the disease
In the case when treatment of the gums during complicated tooth eruption was not carried out, serious complications of the inflammatory process develop:
- Periostitis, or flux, is inflammation of the periosteum.
- Osteomyelitis - in this disease, inflammation affects both the bone tissue itself and the bone marrow, gradually leading to bone resorption. This can cause abnormal jaw fractures.
- An abscess when the infection spreads to nearby tissues. Purulent inflammation leads to the melting of muscles and fatty tissues with the formation of a large accumulation of pus.
- Cellulitis is the next stage of a purulent process after an abscess, which does not have clear boundaries. Such purulent inflammation is a serious threat to the patient and is treated in a maxillofacial hospital.
These complications are usually difficult to treat, require a serious systemic approach and can lead to irreversible consequences. Therefore, if a person suspects he has pericoronitis, treatment should begin without delay in order to prevent the condition from worsening. You need to be especially careful if gum inflammation occurs during teething in children, since the children's immune system is still immature, the body's resistance to infections is lower and the process quickly becomes more severe.
Treatment of periostitis
The main thing to remember is that you cannot try to treat periostitis on your own . There are several actions that absolutely cannot be performed while waiting for a doctor’s appointment, so as not to aggravate the disease:
• apply hot compresses , rinse with soda or drink hot drinks and decoctions. Heat will only increase swelling;
• give painkillers , and even more so antibiotics;
• try to cut the abscess yourself .
Pericoronitis, treatment in children and adults
It should be noted right away that for pericoronitis, treatment at home can only reduce the symptoms of inflammation, but not solve the problem. Therefore, all home methods (rinsing with antiseptics, applying anti-inflammatory ointments, etc.) can only be used as a way to relieve inflammation during the eruption of wisdom teeth and reduce pain - this is a temporary measure before visiting the dentist.
In a dental clinic, in case of complicated teething, treatment will depend on whether the problem tooth should be preserved or whether it should be removed. If preserved, the doctor performs surgical excision of the “hood” under local anesthesia. This eliminates conditions for the accumulation of food and the growth of bacteria, and also facilitates teething. After excision of the “hood,” the patient is prescribed antiseptic therapy (rinses, baths) and, if necessary, antibiotic therapy.
In cases where tooth extraction is indicated due to their incorrect position on the jaw, lack of antagonists, or insufficient space for full eruption, the doctor immediately removes the problematic tooth and prescribes antiseptic therapy to the patient.
In some cases, at the initial stages of the inflammatory process, conservative therapy can be preliminarily applied - local treatment with antiseptic rinses and the introduction of an iodoform tampon into the “hood”. However, local therapy does not always give a positive result; moreover, it is appropriate only at the initial stage of the disease; in other cases, surgical intervention will be required.
When it comes to teething in children, treatment is always aimed at preserving the teeth (except for those cases when dystopia is clearly expressed and the doctor sees that preserving is useless).
There is a lump with pus on the gum - what to do?
If a lump does appear on the gum, you should consult a doctor. In an advanced stage, when discomfort becomes obvious, you should not hesitate with treatment. You will not be able to remove the lump on your own using herbal rinses.
Most often, a neoplasm noticed at the wrong time above a baby tooth causes fear in parents. It seems like something very serious is going on. And sometimes this is true, so do not hesitate to contact the clinic.
The problem can occur anywhere on the gum, mainly above the chewing teeth. The abscess may be red-blue or white-yellow, depending on the cause of its appearance. In any case, you cannot open the abscess yourself, apply ointment, apply compresses, and try in every possible way to cure the gum on your own. This is very dangerous: the infection can spread even further and deeper. It is important to continue your normal oral hygiene routine even if brushing your teeth is uncomfortable.
Diagnostic features
History of the disease Pericoronitis sometimes looks like a completely different disease of the oral cavity - for example, its symptoms can be confused with periodontitis (inflammation of the peri-apical tissues of the oral cavity) or pulpitis (inflammation of the dental pulp). The pain in these diseases is very similar, and periodontitis is often accompanied by hyperemia and swelling of the gums. One disease can be distinguished from another by the following signs: with pulpitis there is no pain when opening the mouth and no noticeable swelling of the gums, and periodontitis develops only at the tops of the roots of fully erupted teeth. You also need to pay attention to the presence of a characteristic “hood” - a photo will help you assess how it looks with pericoronaritis.
Prevention
In some cases, especially when it comes to inflammation of the gums during teething in children, preventive measures will help prevent the disease: careful regular oral hygiene, timely removal of tartar and soft deposits, visits to the dentist for diagnostic examinations at least once every six months.
If pericoronitis is caused by the anatomical features of the structure of the dental system and the lack of space for the lower “eights” on the dental arch, preventive measures will only smooth out the course of the inflammatory process (due to timely cleaning of the oral cavity from bacterial plaque and food particles that create favorable conditions for inflammation) and identify the problem in time (subject to regular dental examinations).
What is pathology
Gingivitis is an inflammatory pathology of the gums, in which there is no damage to the periodontal junction or other periodontal tissues (tissue surrounding the tooth). If treatment does not occur for a long time, then damage to these structures, called periodontitis, may occur. Most often in children, the marginal part of the gum, located next to the dental neck, is affected.
The inflammatory process is promoted by:
- high activity of biological processes in gum tissue;
- formation of the dental system;
- unformed local immunity.
Most often, gingivitis is detected in a child aged 2–4 years, as well as in one-year-old babies during teething.