Darkening of the tooth near the gum can be caused by various reasons. Not all of them are associated with dental diseases and pathological processes in the oral cavity. For example, sometimes a tooth darkens due to taking medications containing iron gluconate, or excessive consumption of grape or tomato juice.
However, in most cases, the causes of darkening of the tooth near the root and gums are pathological processes. This is a reason to immediately contact a dentist. The following diseases lead to this symptom:
- Cervical caries;
- Tartar;
- Fluorosis.
Let's talk about these diseases and methods of treating them in more detail.
Gingivitis: my gums hurt
The process, which is characterized by gum inflammation, swelling, redness and bleeding, is called gingivitis and is one of the most common periodontal diseases in both children and adults. Only 3% of people can boast of absolutely healthy gums. How to get into such a small percentage of lucky ones? The answer is simple - follow the necessary measures to prevent gum inflammation, regularly visit the doctor and not let even seemingly harmless signs of an incipient disease take their course.
Gingivitis is the last of all diseases in periodontology in which the inflammatory process can still be stopped. Next comes periodontitis, a disease in which inflammation spreads to other periodontal tissues. From this point on, treatment is based only on bringing the disease into remission and attempts to relieve symptoms as much as possible at the time of relapses, as well as in the future when it is necessary to resort to tooth extraction. Therefore, gingivitis in children and adults requires increased attention in order to avoid serious periodontal problems.
Questions for the doctor
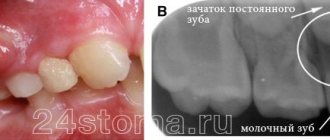
Teething
Tell me, my son has erupted one upper incisor, and in place of the second, the gums have slightly swollen and a dark spot has appeared. Do I need to take any measures or just wait until the tooth erupts?
The appearance of an eruption cyst at the site of a future tooth is a common occurrence. And usually such a cyst goes away on its own, without outside intervention. But to monitor the condition of the child’s teeth and gums, it is necessary to show him to a pediatric dentist.
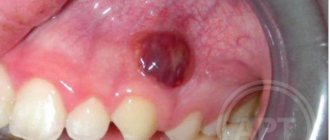
Hematoma on the gum
My daughter has a small black dot under one of her lower incisors. We can see a doctor only in a week. What could this be and does it need to be treated somehow?
If, apart from the black dot on the child’s gum, nothing bothers him, there is no swelling or redness, then most likely this is the result of mechanical damage to the gums from a fall or impact. Such a hematoma usually resolves on its own within a few days, so no additional therapeutic measures are required.
Types of gingivitis
Gingivitis differs in the nature of its course:
- Acute gingivitis is a disease whose symptoms appear suddenly and progress quite quickly.
- Chronic gingivitis is a sluggish process, the symptoms of which increase gradually.
- Aggravated gingivitis (recurrent stage of a chronic process) is an increase in the symptoms of a chronic disease.
- Gingivitis in remission is the moment of complete relief of all symptoms.
The form is:
- catarrhal gingivitis, which is manifested by swelling and redness;
- ulcerative (ulcerative-necrotic) gingivitis, with necrotic (dead) areas of the gums;
- hypertrophic gingivitis, in which there is a significant increase in the volume of gum tissue and its bleeding;
- atrophic gingivitis, on the contrary, is characterized by a decrease in the volume of gingival tissue;
- desquamative (geographic) gingivitis, which is manifested by intense redness and abundant desquamation of the epithelium of the mucous membrane.
According to its distribution in the oral cavity, gingivitis can also be local (affects some areas of the teeth) and generalized (the process affects the gums of the entire jaw or both jaws). And according to severity - mild, moderate and severe gingivitis.
How to deal with little black caries
To prevent the cavity from turning into a large hole, you need to perform remineralization in the dentist's office. To do this, the doctor applies a special composition to the teeth, which quickly penetrates into the deep layers of the damaged units and, as it were, nourishes them from the inside. As a result, the teeth become stronger and more durable, and the rapid spread of the carious process is temporarily blocked.
In case of serious damage, the dentist can give the client a mouth guard and a special remineralizing composition. You need to use all this at night - before going to bed, put the product in a mouth guard and put it on your teeth. Remove in the morning. Repeat the procedure the number of times indicated by the doctor.
Causes of gingivitis
Most often, gingivitis develops as an independent disease, but sometimes the causes of its occurrence are acute and chronic diseases of the gastrointestinal tract, cardiovascular system, hematopoietic organs, infectious diseases, and changes in hormonal levels. In this case, gingivitis is one of the symptoms of the underlying pathology. The causes of gingivitis can be internal or external.
Internal reasons include:
- tooth growth that injures the gums - the eruption of wisdom teeth;
- vitamin deficiency, hypovitaminosis (most often lack of vitamin C and zinc);
- weakened immune system;
- metabolic disease;
- allergic diseases;
- diabetes;
- stress, mental illness;
- anomalies and various deformations of the gums;
- diseases of the gastrointestinal tract.
External reasons are a number of factors:
- physical (injuries, burns);
- chemical (the influence of aggressive substances);
- medical (incorrectly applied fillings, incorrectly installed veneers, traumatic wearing of braces);
- bad habits (smoking, mouth breathing);
- biological (infectious process);
- hygienic (insufficiently thorough hygienic procedures).
Toxins from microorganisms that enter the oral cavity with food and water, as well as those that live there permanently, form dental plaque (plaques) due to insufficient hygiene measures. They are the most common cause of the inflammatory process.
Inflammation can develop differently depending on the cause. Chronic catarrhal gingivitis occurs most often due to unsatisfactory hygiene measures or as a result of gum injury or burns. Hypertrophic gingivitis is caused by crowded teeth, incorrectly installed fillings or dental crowns, as well as changes in hormonal levels, for example, during pregnancy (pregnant gingivitis) or puberty (adolescent or juvenile gingivitis). Necrotizing ulcerative gingivitis (Vincent gingivitis) is usually caused by an infectious process. It occurs due to the activation of two microorganisms (Vincent spirochete and spindle bacillus) against a background of weakened immunity, hypothermia, stress or malnutrition.
Fluorosis
Fluorosis is a dangerous dental disease that is caused by consuming extremely large doses of fluoride. Usually this substance enters the human body along with tap water. In addition, the source of fluoride can be the work environment or even the wrong toothpaste.
Fluorosis begins with the appearance of white, dull spots on the surface of the teeth. They are not always visible to the naked eye. Over time, the spots change color - they first turn yellow, then turn brown. If you don’t consult a dentist at this point, fluorosis can turn into erosive or destructive forms - when the disease begins to destroy the enamel.
Treatment of fluorosis is almost always conservative. The dentist remineralizes the enamel, restoring the balance of calcium, phosphorus and fluoride. Darkened areas are bleached. In addition, the patient is recommended to change his lifestyle to reduce the amount of fluoride consumed - for example, install a special water filter at home or change his place of work.
Fluorosis is often “epidemic” in nature. If it is caused by an increased content of fluoride in tap water, it develops in the whole family. If the reason was a violation of industrial safety - for the entire team. In the Ryazan region, fluorosis is often detected in residents of the Rybnovsky, Chuchkovsky and Shatsky districts, where the water contains an increased amount of fluoride.
Forms of gingivitis and symptoms
Signs of gingivitis directly depend on the nature of the disease and its form. Let's look at each form of gingivitis separately. So, complaints and visual inspection.
Catarrhal gingivitis
This form of the disease usually occurs without obvious pain. Its immediate symptom is bleeding gums when brushing teeth, eating solid foods and other mechanical effects on the dental system.
Ulcerative-necrotizing gingivitis
This is one of the most unpleasant forms of gingivitis, which is characterized by a feeling of itching of the gingival papillae, severe pain, copious flow of saliva, fever, inflammation of the lymph nodes and the formation of necrotic areas of the gums.
Hypertrophic gingivitis
Patients suffering from this form of gingivitis complain of severe pain, constant bleeding of the gums and a significant increase in the volume of the gums, which can partially cover the crowns of the teeth from the outside (not from the tongue). At the same time, the patient’s gum remains quite hard and under it, on the teeth, tartar forms, which creates favorable conditions for the proliferation of microorganisms. With hypertrophic gingivitis, teeth may move slightly.
Atrophic gingivitis
The last and most advanced stage of gingivitis, often leading to periodontitis, is atrophic gingivitis. With it, the gum tissue becomes thinner, decreases in size, the necks of the teeth, and sometimes their roots, are exposed. Teeth become more sensitive to temperature changes (cold or hot drinks, frosty air), to sour or sweet foods, to the mechanical impact of a toothbrush.
Desquamative (geographic) gingivitis
The symptoms of this form of gingivitis differ from others by pronounced red spots on the gums, desquamation of the upper layer of the epithelium, the appearance of blisters on the gums and the formation of mouth ulcers and erosions.
Professional help
Treatment begins with diagnosis and determining the causes of the pathology. After eliminating the causes that provoke the darkening of the enamel, appropriate treatment is prescribed.
The method of treating cervical caries depends on the stage at which the pathology was noticed:
- At the dark spot stage, remineralizing therapy is used: the tooth is cleaned of soft plaque and hard dental deposits, and the affected area is covered with an application containing fluoride.
- In case of superficial and medium caries, the affected area is prepared, after which the tooth is filled.
- At the stage of deep caries, as a rule, the pulp is removed and the canals are cleaned. After this, the tooth is filled.
Diagnostic tests
- Schiller-Pisarev test
This test is based on determining the level of glycogen in the gum. Its amount increases significantly during inflammation, while healthy gums do not contain glycogen. Lubricating the inflamed gums with Schiller-Pisarev solution gives a color change reaction from light brown to brown. This research method is used to make diagnoses of both periodontitis and gingivitis.
- Assessment of oral hygiene level
A solution (2 g of potassium iodide, 1 g of crystalline iodine, 40 ml of distilled water) is applied to the outer surface of the six lower front teeth.
The assessment is carried out using a five-point system and each tooth is assessed separately:
- 5 points – complete staining of the entire tooth surface;
- 4 points – staining of ¾ of the tooth surface;
- 3 points – staining of half the tooth surface;
- 2 points - staining of a quarter of the tooth surface;
- 1 point - absence of any staining of the tooth surface.
Then the scores of all examined teeth are summed up and divided by their number (usually the test is carried out on six teeth). This is how the hygiene index is obtained.
As a result, the quality of hygiene is assessed:
- 1.1-1.5 points – good hygiene index;
- 1.6—2.0—satisfactory hygiene index;
- 2.1—2.5—unsatisfactory hygiene index;
- 2.6—3.4—poor hygiene index;
- 3.5-5.0 - very poor hygiene index.
- Vacuum test according to Kulazhenko
Using a Kulazhenko vacuum apparatus, it is possible to determine the time of hematoma formation when a vacuum is applied to the gum area. Typically, the test is carried out in the incisor area by placing a tube of the device on the gum. The formation of a hematoma in 60 seconds indicates the normal condition of the gums, while the appearance of a hematoma in 29-30 seconds signals an inflammatory process.
- Oxygen tension in gum tissue
The sensor of the device is applied to the gum, and the device records the level of tissue hypoxia. Reduced oxygen tension indicates a prolonged inflammatory process.
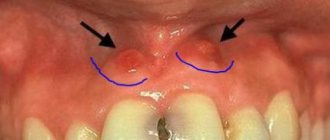
What is epulis
A tumor on the gum is characterized by a benign nature. It is classified as a group of periodontal diseases. Epulis is also called “giant cell granuloma” or “supragingival”. Epulis looks like a lump that is attached to the gum in the area of the interdental space on a stalk. A formation is formed from the epithelium of the alveolar process.
In diameter, an epithelial tumor of the gums can reach a size of more than 3 cm. The shade of a giant cell granuloma can be different: bluish, brown, red-brown, or the color of the gums. Ulcers may appear in the affected area.
If the epulis on the gum has a diameter of up to 2 cm, does not cause pronounced symptoms and progresses slowly, then the pathology is classified as a benign form. With rapid growth of the supragingival tissue, severe pain, inflammation and swelling of the gums, there is a risk of developing a malignant tumor.
According to statistics, the pathology is most often diagnosed in pregnant women, but supragingival formation also occurs in women who are not pregnant. Less commonly, the disease occurs in men and young children when replacing milk teeth with permanent ones.
Differential diagnosis of gingivitis
It is based on the complaints presented to the patient, a visual examination of the patient, the results of functional tests and laboratory tests. The goal of differential diagnosis is to distinguish gingivitis from other periodontal diseases, such as periodontitis and periodontal disease.
The main feature that distinguishes gingivitis from other periodontal diseases is that the inflammatory process affects only the gum tissue, the remaining structures (muscle ligaments that hold the tooth in the jaw and bone tissue) remain unchanged.
Along with this symptom, gingivitis is not characterized by periodontal pockets, exposure of the necks of teeth, or their mobility. And the x-ray shows no signs of bone resorption.
Identifying gingivitis in a timely manner, determining its form and prescribing the correct treatment is the task of a periodontist. But not to forget about prevention and regularly visit the dental clinic is the maximum program for the patient. This is the only way to avoid a more serious periodontal disease – periodontitis.
Treatment of a darkened tooth
Darkening of the tooth near the gum requires immediate consultation with a doctor, regardless of the cause. If you leave the disease to its own devices, you can face more dangerous and serious consequences.
The doctors at our regional dental clinic are ready to help. We use modern equipment, progressive therapeutic practices and always put the patient's comfort as a priority. Therefore, treatment of a darkened tooth will be quick and effective. Don’t let the disease lead to dangerous consequences - make an appointment with the dentist!