1. Lipomas
Formations on the genitals come in several varieties. The reasons, patterns, mechanisms of their occurrence in some cases are known and understandable, in others they remain not entirely clear. Different types of formations affect specific tissues. The following types of formations on the external genitalia are divided: lipoma, atheroma, bartholinitis, papilloma.
Lipomas
most often form in the subcutaneous fat layer. It is impossible to clearly identify the reasons for their occurrence, but a certain statistical connection with hereditary predisposition has been established. Moreover, the growth of lipomas has nothing to do with fat consumption or a tendency to develop subcutaneous fat deposits. The incidence of lipomas in thin and overweight people is the same. Lipomas can range in size from 1 to 15 cm and are usually not painful or itchy, presenting only a cosmetic problem. Cases of malignant degeneration of lipomas are very rare; More often, mechanical damage carries the threat of suppuration and infection. Lipomas up to 3 cm are treated non-surgically - by injecting them with a drug, the action of which leads to the resorption of the formation. Large lipomas are removed surgically: with laser, electrocoagulation or radioknife.
As a rule, a new lipoma does not appear at the site of a well-performed operation. However, it is not uncommon for new lipomas to form in nearby tissues.
A must read! Help with treatment and hospitalization!
Treatment of white spots
If white spots appear on the genitals, including the labia, then this is a direct indication for examination and comprehensive treatment of the patient.
Women, when problems appear on the labia, do not always have a clear idea of where to go to get diagnosed and take all the necessary tests.
Which doctor deals with these problems?
As a rule, it is better for a woman to visit an examination room at a local clinic or make an appointment with a gynecologist.
Depending on the results obtained, the patient will be treated by a gynecologist, dermatovenerologist, allergist, endocrinologist or oncologist.
Timely diagnosis carried out by a specialist and tests that will need to be taken to find out the cause of the disease play a decisive role in the effectiveness of treatment.
How treatment will proceed depends on the cause of the disease.
Drug therapy is used, and in some cases surgery may be necessary.
- If the appearance of rashes is caused by ignoring the rules of personal hygiene, then it will be enough to follow them with the mandatory inclusion of water procedures and the use of hygiene products containing antiseptic components. If white spots appear as a result of heat rash, using baby powder with zinc will be enough.
- If the pathology has developed as a result of infection with pathogenic flora, then specific therapy will be required. A treatment regimen for the disease will be drawn up by a doctor based on the results of additional research and the stage of the disease.
- If there is no evidence of an infectious process, the doctor may recommend treating the rash with a disinfectant.
- If there is an allergy, then taking an antihistamine will be an ideal assistant in solving the problem; in case of hormonal imbalance, corticosteroids will come to the rescue, which should be prescribed by a specialist.
Regardless of the cause of the appearance of white spots in an intimate place, it is useful to take immunomodulators and vitamin-mineral complexes that will help the body cope with the pathology.
2.Atheromas
Atheroma
is a cyst filled with a yellowish fluid formed by fat cells, epidermis and sebum. Since all this in the cyst is in a state of stagnation, when opened, the substance that is usually removed has an unpleasant odor. Causes of atheroma: increased oily skin, acne, poor cleanliness, hormonal changes, heredity. Atheromas form where there are many sebaceous and sweat glands. When they grow to a size of 5 cm, tension occurs on the surface of the skin and even internal inflammation is possible. It is always recommended to remove atheromas without waiting for complications, although they also degenerate extremely rarely.
The atheroma is completely removed by isolating it from the tissue. At the same time, they try not to disrupt its integrity and make sure that no particles of the cyst shell remain, otherwise this may cause a relapse in the same place.
Visit our Gynecology page
Surgical methods for removing formations on the labia
In some cases, they resort to surgical removal of formations in an intimate place.
Indications for it are:
- the presence of papillomas and genital warts;
- fatty cysts;
- the appearance of neoplasms;
- presence of subcutaneous acne;
- molluscum contagiosum;
- furunculosis;
- inflammation of the Bartholin gland.
Most often, minimally invasive removal techniques are used: cryodestruction, laser therapy and radio wave excision of elements.
In exceptional cases, surgery can be performed using a scalpel.
- Laser therapy - this method is based on the use of a laser beam that evaporates the contents of the tumor. The technique is used to remove papillomas, cystic formations, and elements of rash caused by molluscum contagiosum.
- Radio wave therapy – the effect of radio waves is similar to the effect of a laser beam. The technology is used for excision of tumors.
- The use of liquid nitrogen (cryodestruction) is used to remove papillomas, molluscum contagiosum rashes, and condylomas. The method is rarely used due to the impossibility of controlling the depth of freezing of elements.
- Diathermocoagulation is a method that is very rarely used to excise tumors localized on the labia, since there is a high risk of burning surrounding tissues.
- Surgical intervention is used in case of a large size of the element or if its malignant nature is suspected.
After removal of the formation, a histological examination of the material is required, which is important to determine its benignity or malignancy.
3.Bartholinitis
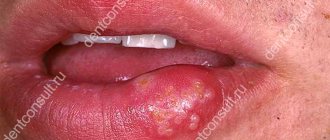
Bartholinitis
- This is a consequence of blockage of the Bartholin gland. It is located at the entrance to the vagina and is involved in lubrication (moistening) of the external genitalia. During moments of sexual arousal, this process is especially intense. When a blockage of the gland duct occurs, a cyst is formed in which the produced secretion accumulates. If therapeutic measures are not taken, infection and cyst rupture often occur. This gives relief because the cavity is freed from accumulated secretory masses. However, the consequences of such spontaneous opening against the background of an abscess can be very dangerous. You should definitely consult a doctor at the first sign of a lump at the entrance to the vagina. If treatment is not carried out or the cyst does not open spontaneously, general malaise begins: the temperature rises, pain is felt when walking, and signs of acute infection appear. In the most difficult cases, the abscess can spread to the internal genital organs: the uterus, appendages.
Treatment of bartholinitis in uncomplicated cases by opening the cyst is not difficult. The operation is performed on an outpatient basis under local anesthesia. In more severe cases or when a postoperative relapse is established, a decision is made on bartholinectomy (complete removal of the Bartholin gland). This is a rather complicated operation, but in some cases it cannot be avoided.
About our clinic Chistye Prudy metro station Medintercom page!
Drug treatment of white spots on the genitals
- If there are rashes on the genitals, medications are used to help normalize the vaginal microflora. For this purpose, solutions, vaginal suppositories and vaginal tablets are used to help get rid of pathogenic microorganisms.
- In case of viral infection of the intimate area, tablets or injections are prescribed. The duration of drug treatment is determined by the doctor. On average it ranges from 10 days to two weeks. If herpetic rashes appear on the genitals, then ointments containing an antiviral active ingredient are used. If papillomas are present, they can be treated with keratolytics.
- For furunculosis, ointments with an osmotic effect are used, which accelerate the process of maturation and opening of the abscess.
- If an allergic rash occurs, you will need to identify the allergen that triggered its appearance and prevent skin contact with it. To relieve itching, your doctor may recommend taking an antihistamine.
4. Papillomas
Papillomas
external genitalia - this is the growth of the epidermis of the labia. By their appearance, papillomas are easily differentiated from other formations. They are usually located on a stalk, resembling the shape of a mushroom. Unlike other uncomplicated formations, papillomas may itch or hurt; They are often injured. The reason for their appearance is HPV, the human papillomavirus, which is activated under favorable conditions (decreased immunity, stress, hormonal changes). HPV infection occurs through sexual contact or from the mother at birth. The latent period of this virus (without any formations on the skin) can last indefinitely. The actual growth of the epidermis on the genitals can be provoked by a number of factors, mainly associated with a decrease or depletion of the body's protective resources.
Papillomas are always treated comprehensively: formations on the skin are surgically removed, and the human papillomavirus itself is subjected to systemic therapy aimed at increasing immunity, restoring hormonal balance and balanced metabolism.
It is necessary to treat papillomas. Not only can they grow to large sizes, but they also carry the risk of infecting a sexual partner.
White dots: causes of appearance and location of localization
The labia are abundantly supplied with hair follicles and glandular cells.
Sex hormones actively influence the activity of the glands.
The appearance of white spots on the skin and mucous membranes of the genitals can be caused by:
- blockage of glandular ducts;
- development of the infectious process;
- cystic formations in the ducts of the glands. The resulting wen (lipomas) in the absence of an inflammatory process in them are considered harmless. They are a benign form. Lipoma on the labia is painless and mobile. There are: fibrolipoma, angiolipoma and liposarcoma. Lymphosarcoma is a malignant form and tends to metastasize. The presence of cysts may indicate a weak immune system;
- infection of the hair follicles (folliculitis).
- White spots that form under the skin or in the thickness of the labia majora require mandatory consultation with a specialist. They can be caused by an infectious process or hormonal changes;
- when the formations are localized inside the labia on one side, it may mean inflammation of the Bartholin gland or be a sign of the formation of a boil;
- degeneration of tissues into a malignant form;
- changes in hormonal balance.
If white dots appear on the labia minora or majora and they cause concern, then we may be talking about a pathological process.
In this case, you will need to undergo additional research and consult specialists.
Symptoms of the disease and its danger
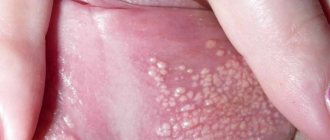
Fox Fordyce granules on the female intimate organs look like papules, nodules or spots of yellow, white, cream color. They are located on the inner or outer surface of the labia minora and majora, in the pubic area, near the clitoris and vestibule of the vagina. Fordyce granules rarely appear on the vagina. They are 1-2 mm in size and are not accompanied by subjective symptoms. The pimples protrude slightly above the surface of the mucosa. On palpation, the surface of the labia is felt to be rough.
Multiple granules are arranged in separate groups in several rows or merge into a single plaque. Solitary Fordyce formations in the genital area are less common. When pressed, their color does not change.
When contacting a dermatologist, the diagnosis is established on the basis of medical history, localization and the absence of subjective sensations in the lip area. In doubtful cases, a histological examination of the formations is carried out.
Fordyce granules on the labia minora in women are not dangerous. They are safe for the wearer and his sexual partners. Nodules are not transmitted through household contact, since the pathology is associated with the anatomy and physiology of a particular person, and not with an infectious factor.
Treatment for Fox-Fordyce granules in the female labia area is not required. It is indicated only at the personal request of the patient.
However, the appearance of nodules can be combined with disruption of the apocrine sweat glands. In this case, Fox and Fordyce disease develops. A blockage occurs, causing the ducts to overflow and rupture. The secretion escapes into the surrounding genital tissues, causing inflammation and itching. There is an increase in discomfort in the lip area before menstruation and during pregnancy. The disease has a chronic course with periodic exacerbations. Treatment is mandatory.
Hygiene procedures for white spots on the labia
If the appearance of white spots on the labia is associated with poor hygiene, then washing the genitals daily with baby soap will help get rid of the problem.
Treatment procedures using antiseptic agents are usually prescribed by a gynecologist or dermatovenerologist.
In addition, some rules should be followed:
- when choosing underwear, make sure that it is made from natural fabrics;
- refuse to wear thong panties;
- Avoid using pads that contain fragrances, as they can cause rashes;
- use only a personal towel for hands, face and body;
- exclusion of hair removal and means for its implementation on the labia majora;
- When visiting a bathhouse or swimming pool, strictly observe hygiene rules.